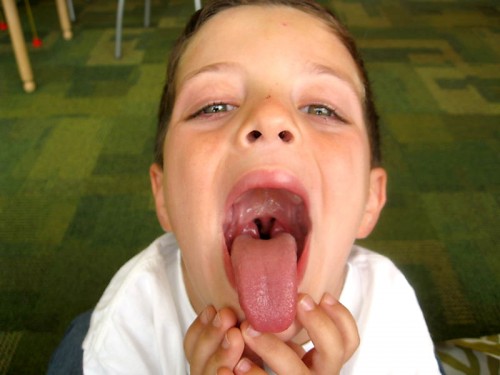
Tonsillectomy – part two
Due to editing and space constraints, my (newspaper) article on tonsillectomy two weeks ago did not present the entire picture of how physicians feel about this surgical procedure… and generated several additional questions – which we will cover here.
Nonexudative pharyngitis, normal tonsils
Although tonsils and sore throats are just little things, several concepts should be carefully understood.
After all, it is the second most frequent surgery performed on children in any area. And hundreds of thousands of dollars are spent in every community on this one surgical procedure alone — including ours.
The recent questions raised included: “What if Johnny had a lot of sore throats, but they weren’t Strep?”, “What if it’s tonsillitis?”, “Is tonsillitis contagious?” “What tonsillitis symptoms should I look for?”, “What is chronic tonsillitis?” and “my friend, who is a nurse, said that child tonsillitis is bad and he should have a tonsillectomy.”
Remember that in this article, we are discussing tonsillitis (actually infected, tonsilar lymph tissues) not pharangitis (painful mucus tissues in the throat); because, the former is the problem which might lead to a tonsillectomy the latter is not.
Tonsils are a collection of lymph tissue whose job it is to help fight off infection. There are lymph nodes found under the skin all over the body and they increase in size during local infections; then, decrease back to normal as their work of filtering infected tissue juice is done. You don’t cut something out just because it does its job!
The normal, average, healthy ten year old has had, on the average, one hundred illnesses! Some have more, some less; but, according to careful studies, a child can still be considered healthy and average if he is ill almost one time per month.
Almost every kind of cold, and many allergies, will produce a sore throat along with their illness. This does not mean that the tonsils should come out; nor, does it mean that all sore throats are treated with antibiotics.
Studies show that: if the tonsils are primarily infected themselves with puss on their surface, there are swollen and tender neck lymph nodes and the child has a high fever and foul smelling breath, then there is just over a 50/50 chance that the child actually has a “Strep Throat”. A throat culture (or these days a spot test) is a more accurate way to know for sure – in fact, the only accurate way.
That means then that even the mildly ill child with no puss or significant symptoms might also have a Strep throat! So don’t be fooled. It also means that IF either you or your doctor is considering putting your child through a tonsillectomy; then, throat cultures are the minimum requirement for diagnosis and not too much to ask.
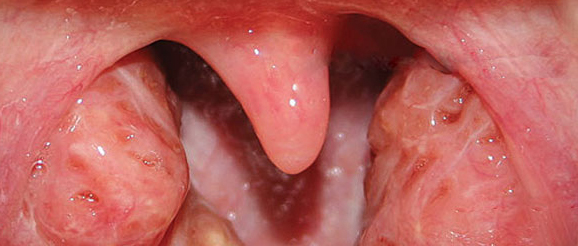 Normal child tonsils, cryptic, do NOT need removal
Normal child tonsils, cryptic, do NOT need removalWhy are we so concerned about Strep throats? Because if it is Strep; and if it is a certain type of Streptococcus; and if it is not treated within 72 hours for a full 10 day course of antibiotics; then the child runs a 5 -15 percent risk of developing rheumatic heart disease.
You might say “Well if, if, if, then doesn’t sound too significant;” and that would be true – for one time. However several of them combined become significant and that’s why physicians then elect to take the tonsils out. When the risk of rheumatic heart disease (as low as it is) is greater than the risk of death and morbidity (complications) from tonsil surgery (as low as it is also), then tonsils should come out.
Even then, however, there is no guarantee that the child will have fewer Strep infections, and little evidence that taking the tonsils out even cuts down the number of sore throats.
In addition, an extremely large study (over 600,000 cases) showed a death rate of one child per 16,381 operations. Some may not consider this rate to be very risky; but, it is greater than the risk, in some studies, of crib death and think how serious we take that!
The death rate in tonsillectomy is also much greater than the risk of serious permanent brain damage following Pertussis vaccine. It helps to put things in their perspective.
The death rate in tonsillectomy is also much greater than the risk of serious permanent brain damage following Pertussis vaccine.
So why take tonsils out? Well, that’s my whole point! Most pediatricians, who do not perform the procedure themselves and are therefore at less risk for remunerative bias, agree that there are many more tonsillectomies performed than had probably ought to be, if one followed the evidence based guidelines.
There are situations in which clearly the benefits tend to outweigh the risks and tonsillectomies “ought” to be performed.
As mentioned previously, they are: 1 – cancer of the tonsil, 2 – peritonsillar abscess, 3 – significant and severe airway obstruction which interferes with eating or breathing, 4 – acute tonsillitis so severe that hospitalization is necessary, and 5 – recurrent streptococcus tonsillitis.
There are some “philosophical indications” for tonsillectomy, however. Many physicians feel that a patient having four or more episodes of tonsillitis (not just pharyngitis) a year, for at least two years and necessitating their missing ten or more days a year of school or work will benefit from a tonsillectomy.
However, these decisions should be made in consultation between you and your child’s pediatrician.
It is probably better to discuss the case with, or ask for referral from, a pediatrician prior to seeing a surgical specialist.
2 Posts in Tonsillectomy (tonsillectomy) Series
- follow-up and clarification – 25 Apr 2015
- Indications for surgery – 21 Apr 2015
Advertisement by Google
(sorry, only few pages have ads)