Swaddling and Hip Dysplasia
Besides probing around in ears, for a pediatrician, feeling an infants cranial sutures (soft spot) and checking an infants hips for dysplasia comes about as second nature to them as breathing air.
I even find myself doing it subconsciously when somebody shows me their baby at church – it just comes so second-nature that I find my hand feeling along the top of the baby’s head before I realize what it’s doing.
It’s the hips that I’d like to take a few moments to update you on today and it involves a fairly universal custom – that of swaddling. It turns out that there is a RIGHT WAY and a WRONG WAY to do it – and many of us have been doing it wrong to the hurt of a sizeable percentage of infants.
Swaddling
Bundling babies in blankets with arms restrained and legs extended, either with or without a board or cradle, we now know serves to actually promote the dislocation of a baby’s hips!
This recent knowledge comes just at a time when there has actually been a resurgence in the practice due to finding that: “in general swaddled infants arouse less and sleep longer and that preterm infants show improved neuromuscular development” when they are swaddled (Pediatrics 2007;120:e1097–106).
As usual, fanatics and entrepreneurs expanded and embellished the truth of what was said to claim that it also helped colic in order to sell more swaddling devices. This is just as much a problem as the “bad” swaddling. Recent studies are showing that “there is NO scientific base for the use of swaddling in the treatment of colic”. And an ordinary baby blanket is all you really need to do the “good” swaddling, definitely NOT any “special” (and expensive) swaddling blanket or contraption.
Approximately 90 percent of North American infants are swaddled in the first few months of life. So, there is much more risk in giving an infant what is called “developmental dysplasia of the hip (DDH).” That’s when the “ball” of the upper leg doesn’t seat firmly and solidly inside the “socket” of the hip.
Hip Dislocation and Dysplasia
Good pediatricians ALWAYS examine every infants hips every time they get a chance; because, there is such a sizeable percentage of hips are “loose” (about 20 percent by screening ultrasound) and therefore at risk for complications, that we need to institute therapy as early as we can.
A study in Norway revealed that hip dysplasia accounted for 20% of total hip replacements in patients under 40. A study in Turkey showed a statistically significant relationship between swaddling and hip dislocation. Animal studies show worsening dysplasia the longer the practice continues.
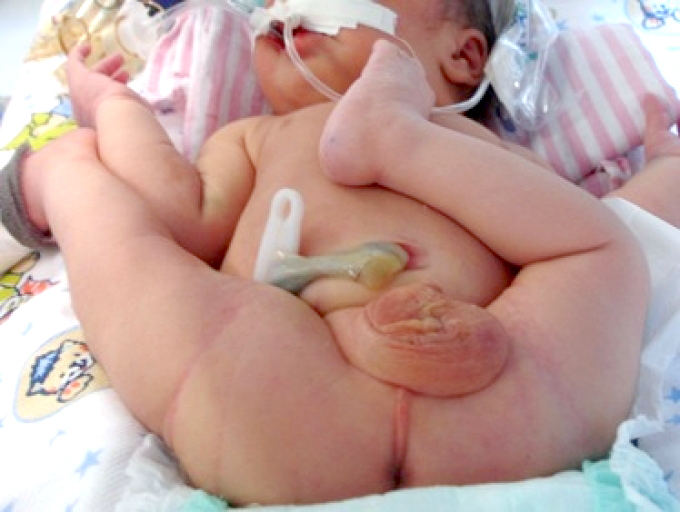 A high incidence of hip dislocation is seen in Native American infants who are placed on traditional swaddling boards; and a huge educational program in Japan taught grandmothers to prevent traditional swaddling, which brought the nations incidence of dislocated hips from as high as 3.5% down to only 0.2 percent.
A high incidence of hip dislocation is seen in Native American infants who are placed on traditional swaddling boards; and a huge educational program in Japan taught grandmothers to prevent traditional swaddling, which brought the nations incidence of dislocated hips from as high as 3.5% down to only 0.2 percent.
A study in Australia showed the opposite side of the coin – over the study time they noted a 300 percent increase of dislocated hips in one institution and the authors attributed it to the resurgence in the swaddling practice. Demand for swaddling clothes increased by 61% in the UK in 2011!
It is normal for an infant who has been “packaged” in a womb for 9 months to have flexion contractures of the hips at birth, up to 28 degrees. And none of the joints are fully formed yet, it’s not limited to just the hips. We’ve already said that 20% of all infants have actual hip dysplasia or acetabular (socket) growth retardation in the first month of life.
In most cases, all of the post-birth freedom of their limbs allows those contractures to resolve to less than 19° at 6 weeks of age and to 7° by 3 months – that is unless other environmental factors intervene like swaddling, which forces the hips into extension and adduction (pulling them next to each other.)
Of course there are other risk factors like breech delivery and family history, but we now are understanding just how important other mechanical factors are as well.
Early diagnosis leads to relatively simple and successful treatment with splints. Only occasionally is surgery necessary.
The Rest of the Story
What can you do? First, make sure that your newborn gets several good physical examinations. You can tell if your doctor is examining the hips just by watching. He’ll have the baby pretty much undressed and manipulate each leg in turn while holding the other side firmly in his hand at the pelvis. It sometimes isn’t too comfortable for the baby.
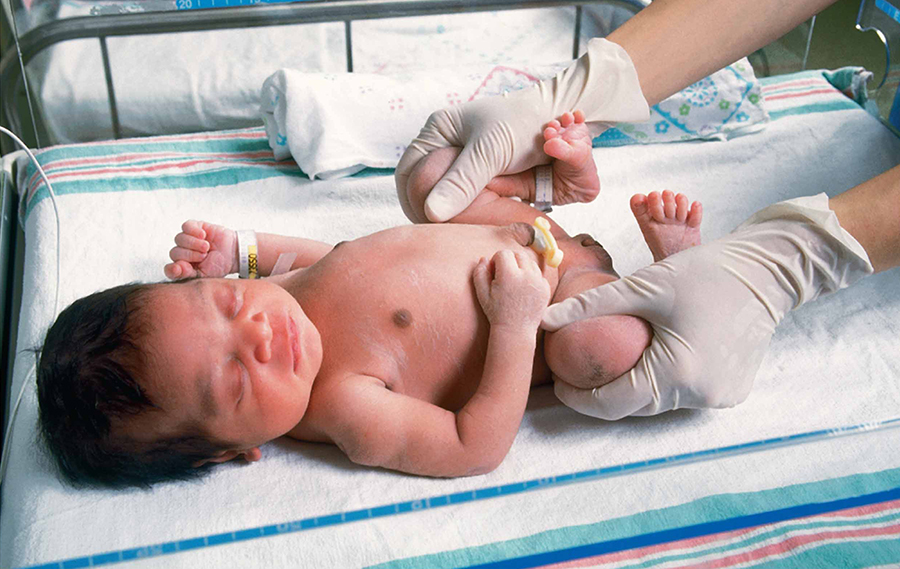 If they don’t do it at each well baby visit, ask them. They should be able to tell you if they felt the normal laxity and how it’s tightening up or if they felt any “clicks” when they did the maneuvers. If they have any questions about their findings on the exam they will want to order an ultrasound to delineate the problem.
If they don’t do it at each well baby visit, ask them. They should be able to tell you if they felt the normal laxity and how it’s tightening up or if they felt any “clicks” when they did the maneuvers. If they have any questions about their findings on the exam they will want to order an ultrasound to delineate the problem.
Second, learn and use what they now are calling “safe swaddling.” All that means is to snuggle the arms and chest with the blanket but allow the legs full flexion at the waist and only wrap them loosely. We’re not calling for you to succumb to the hysteria and go purchase new swaddling equipment, bedding and clothing. A baby blanket is just fine.
Third, we’re also not saying that the baby can NEVER have her legs together, just not habitually for longs periods of time. So, check your equipment like infant carriers, car seats and the like to make sure that its padding doesn’t continually squish the legs into adduction.
You don’t need to go buy new equipment if it does. Just remove some of the excess padding OR just use it for short periods and not make the baby live/sleep in it.
And Fourth, spread the word. Japan had great success with their program for grandmothers. Make sure all care-givers are on the same page and know how to “safe swaddle.”
What we’re trying to do is allow the infant the opportunity and ability to move to the “fetal position” whenever they desire, with the legs up and out, for the first 6 months of life.
I’ll place a short video below which shows the several different ways to do “safe swaddling” with a normal baby blanket.
[Arch Dis Child. 2014;99(1)]
Advertisement by Google
(sorry, only few pages have ads)

