Scabies in Children
I once heard a tape of an old-time radio broadcast where Costello was telling Abbot that “I once had the seven-year-itch.” Abbot asked, “Well, what did you do?” to which Costello replied, “I scratched real fast and got rid of it in four years.”
The seven-year itch was given its nick-name not because it lasts for seven years but because it occurs in epidemics nearly every seventh year.
Didn’t We Already Eradicate Scabies?
Heavens no! It’s still around and thriving. The correct name for the seven-year-itch is scabies, and it is caused by a burrowing mite.
The tiny microscopic animal with pincers comes in contact to the skin where it begins invading and burrowing. The female lays eggs all along the burrow and more mites develop. They burrow to other locations causing intense itching.
It is still epidemic in the United States and highly contagious. The first time an individual is exposed to the mite, there may be a small red rash at the point of entry.
The full-blown disease with rash and the intensive puritis (itching) occurs approximately four to six weeks later when the body has developed some immunity against the mites.
This immunity then causes a hypersensitivity reaction where the skin welts and pus cells infiltrate the area causing swelling. There may be hundreds of itching papules (scabs) along just several burrows.
Diagnosing Scabies
 From a physician’s standpoint, the diagnosis can be very easy or very difficult, depending upon whether the physician is used to seeing the problem (after 7 years absence, you intend to forget about it); and whether or not the patient has done any “self-treating with steroids.”
From a physician’s standpoint, the diagnosis can be very easy or very difficult, depending upon whether the physician is used to seeing the problem (after 7 years absence, you intend to forget about it); and whether or not the patient has done any “self-treating with steroids.”
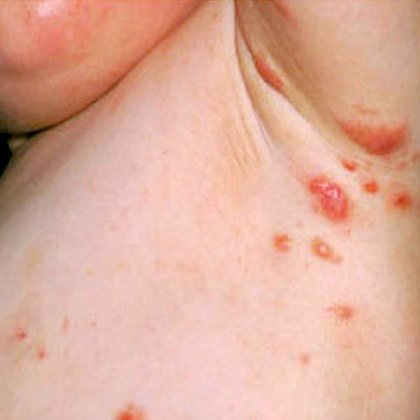
In older children and adolescents, the scabies lesions tend to involve the webs of the fingers, the axillas (armpits), the flexures of the arms and wrists, the belt line, and the areas around the nipples, genitals and lower buttocks.
In infants, however, there is more likely to be involvement of the trunk, extremities, head, neck palms, and soles.
Usually by the time the physician sees the illness there is, in addition, scratch marks surrounding of the skin, making the diagnosis difficult.
There may be blistering and crusting, which might be caused by a secondary infection of bacteria which has come on top of the scabies.
Occasionally, the red, raised rash is in a linear fashion along the burrow of the mite. When this is seen, the diagnosis is easy but they only occur in 7 to 12 percent of adolescents and even less in children.
No matter how the disease presents, the hallmark is intense itching. It is readily transmitted throughout the entire household by skin-to-skin contact with infected persons, especially bed partners.
Spreading by clothing or bedding is supposed to be a less significant risk but still happens frequently enough to still be considered in treatment/prevention decisions.
For diagnosis a burrow may be difficult to find because it is obscured by scratch marks or secondary rashes. If no burrows are found on the fingers, wrists, and male genitalia, the entire skin surface should be examined.
Once a likely burrow is found the diagnosis is made by a skin biopsy or by “scraping.” Some microscope oil is placed on a new lesion and the skin is scraped with a scalpel blade.
The oil is then wiped onto a microscope slide and it is examined for presence of the mites or their body parts, eggs or feces.
Treatment of Scabies
 Diagnosis is most difficult when steroids have already been used in a “shotgun” fashion to treat itching because steroids are powerful hormones which suppress the body’s normal immunity and mask the symptoms of the disease.
Diagnosis is most difficult when steroids have already been used in a “shotgun” fashion to treat itching because steroids are powerful hormones which suppress the body’s normal immunity and mask the symptoms of the disease.
When this article was first written I said that “treatment had become a little controversial”. It is less so now.
One drug, Lindane, was most effective and cured 96 percent of cases with ONE six-to-eight-hour application. But it, along with sulfur ointment, is mainly of historical interest now because it was eventually found to be potentially neurotoxic. So it is avoided in infants and small children.
Treatment with a topical (scabicide) cream usually works if it is applied thoroughly to all skin from the neck down, particularly the finger webs, genitalia, perianal areas, and toe webs. And if it remains on the skin for at least 12 hours, preferably 24 hours, before it is washed off.
The cream containing 5% permethrin is often used first because it is safe for all age groups. But improvement is slow: the itching takes 1 – 2 weeks to subside and the rash 1 – 2 months.
After the diagnosis is made then steroids can provide some relief which could prevent “overtreatment” because a person doesn’t think they are all better.
Remember, in order to prevent re-infestation it is important that all skin-to-skin contacts (eg, all family members, “close” daycare and school contacts and “social” contacts) should be treated at the same time. And, although the mite doesn’t live long off the human body, bedding and clothing should be cleaned; possibly a few times during treatment phase.
There is an experimental drug, Ivermectin, which is purported to cure scabies with one single oral dose. It may prove to be useful, but undoubtedly will be priced to be more than the cream.
Advertisement by Google
(sorry, only few pages have ads)