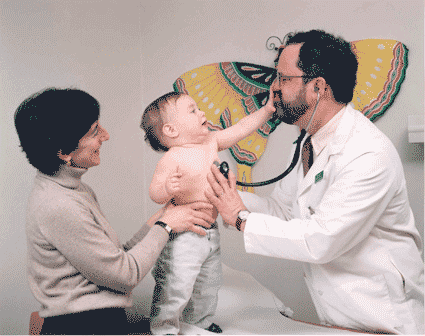
Hospitalized Newborns – One
A residency is basically two to five years in which a physician lives in the hospital.
In the case of a pediatrician, it is three years trying to learn the sum total of the current knowledge about children – and believe me that there’s enough and to spare.
Nearly all of the learning takes place within the small area comprising the approximately 50 – bed pediatric unit and pediatric clinic.
It is a time in which priorities have to be rearranged, and consequently, it is very difficult to do some simple courtesies like writing home.
One technique that I used, late in my on-call night when things had quieted down somewhat, was to take a tape recorder on my rounds and record a letter.
Using that technique, let me take you with me on my hospital rounds. (These are a composite of actual cases in which names have been changed.)
We try and begin our rounds in the nursery for hospitalized newborns, so as not to carry any more germs into it than necessary from the other patients.
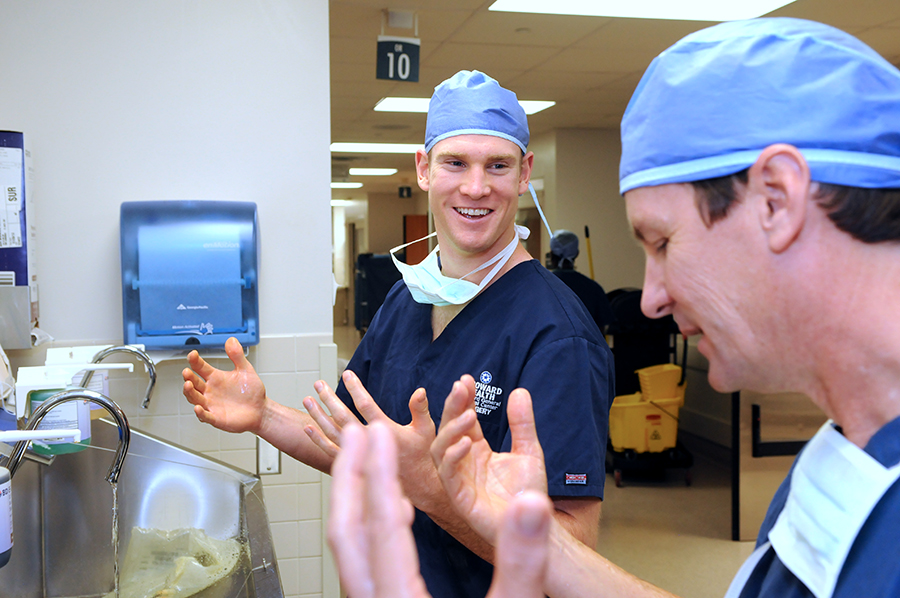 While scrubbing up at the sink, I meet a colleague of mine and tell him of the baby I admitted to pediatrics last night with meningitis.
While scrubbing up at the sink, I meet a colleague of mine and tell him of the baby I admitted to pediatrics last night with meningitis.
The lab results this morning showed that it was bacterial, a germ known as Hemophilus Influenza. This makes sense because we have seen a lot of other illness around the community this week caused by that organism.
He tells me of a phone call that he had last night from a patient who claimed to be one of mine.
It was a man caller who described diarrhea in his child and was fairly insistent on having some paregoric called in.
I told him I didn’t recognize the name but had heard that another doctor had had a similar call.
It is a habit of most of us not to call in paragoric prescriptions as there are people who call around to pharmacies and doctors for the opium content in paragoric (paragoric is tincture of opium).
You might think newborn care is pretty much routine, but today we have four babies all with different histories.
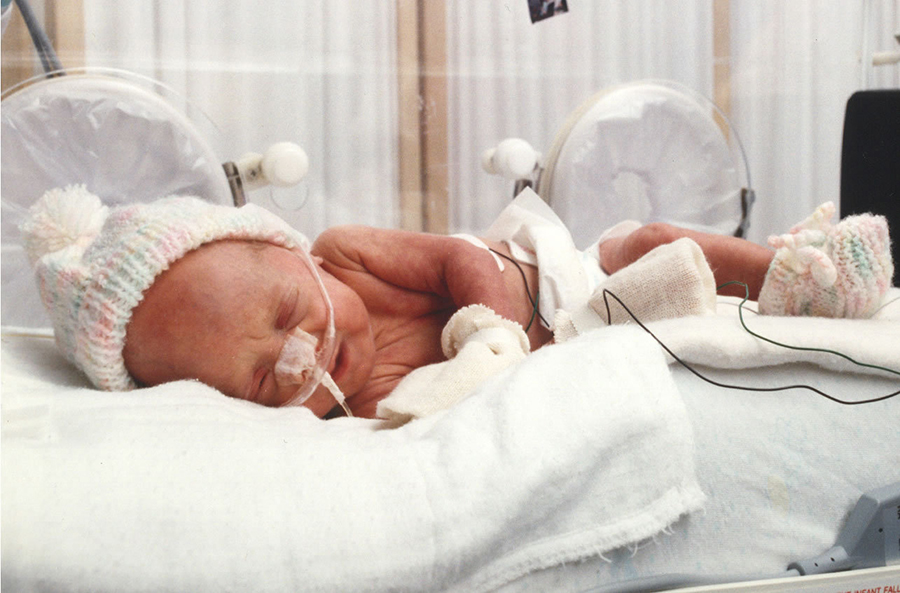 Little Aaron was born one-month premature. He’s been taken care of by a neonatologist (a pediatrician who likes living in the hospital and deals only with critical care of premature infants).
Little Aaron was born one-month premature. He’s been taken care of by a neonatologist (a pediatrician who likes living in the hospital and deals only with critical care of premature infants).
He spent the first week on a respirator but now has been transferred to the “growing nursery” under my care.
He still needs quite specialized care, and we are watching him gain enough weight so that he can maintain his own body temperature and move out of his isolette “house” and into an open crib.
He is a slow feeder, and the nurses spend a great deal of time “coaxing him” to eat.
I will write an order to begin iron drops which we will continue for several months, because much of a baby’s body’s iron is stored in the last trimester, which Aaron has missed out on.
 Erin was born early this morning. She is doing well, but her mother desires a hospital “short-stay” (under 24 hours).
Erin was born early this morning. She is doing well, but her mother desires a hospital “short-stay” (under 24 hours).
The vast majority of infants going home on short stay do very well, but I must confess that it makes me somewhat uneasy.
Every pediatrician knows that there are many significant problems that cannot be picked up on the first examination. Some can come on very quickly, and a few can even be fatal.
For example, most heart murmurs are not head for the first few days or months of life.
Jaundice doesn’t usually begin until the third day, nor do some infections.
Because this is Erin’s mothers first time through, she will miss out on all of the teaching from the nurses, which is a problem because the mother is 17.
I’m going to give her my infants health care manual and I’ll also ask a home nurse to visit tomorrow. I’ll see her in my office on the third day of life.
 Airen’s mother had toxemia, and during labor her heart rate had dropped drastically because her umbilical chord had come down into the birth canal before her head. Every time there was a contraction, the pressure cut off the baby’s blood supply.
Airen’s mother had toxemia, and during labor her heart rate had dropped drastically because her umbilical chord had come down into the birth canal before her head. Every time there was a contraction, the pressure cut off the baby’s blood supply.
Her life was literally saved by being born in the hospital where fetal monitors picked up the problem early, labor could be stopped, the baby’s head held up off the cord, and an emergency C-section could be performed.
Her lungs, however, did not get that final “squeeze” to remove the amniotic fluid from her lung and she has and a short course of transient tachypnea of the newborn (TTN for short).
We put her under oxygen for a few hours, and her breathing dropped from about once a second to about 30 times a minute.
She is doing well now, and her mother wants to take her home today, so I’ll dictate a discharge summary.
 Little Ahran was delivered three days ago. Her mother is ready to go home today, but the nurses tell me that she has developed a cold sore on her lip.
Little Ahran was delivered three days ago. Her mother is ready to go home today, but the nurses tell me that she has developed a cold sore on her lip.
When I go out and talk to Ahran’s mother, I will need to tell her how extremely dangerous herpes infection (the virus which causes cold sores) is in a newborn.
If contracted in the neonatal (under two months old) period, the virus can, in some cases, rapidly spread throughout the body, causing infection and possibly meningitis.
We’ll have her wear a mask and wash her hands very carefully and wear latex gloves when touching Ahran. She’ll need to not kiss Ahran until her lesion has completely healed over. Ouch!
Babies who are over two months old still may get ill from cold sores, but they seem to be better able to fight off the infection.
As I leave the nursery, the head nurse asks me about my “vote” on a food company’s request to hand out samples of their product to mothers of newborns.
It is a dried cereal and vegetable product which has powdered formula mixed in with it!!!
This particular mixture doesn’t have the same quality formula in it as does Enfamil or Similac, and I told her I thought it inappropriate to be giving this type of product out in the nursery. We don’t start babies on cereal until much later and vegetables even later than that – let alone giving them to a new born.
Apparently this company is trying to do an “end run” around all the pediatricians in town who have already told them that “they absolutely would not endorse giving this formula to newborn babies.” Even for older babies – there is absolutely no need to give babies formula and cereal mixed together in a bottle.