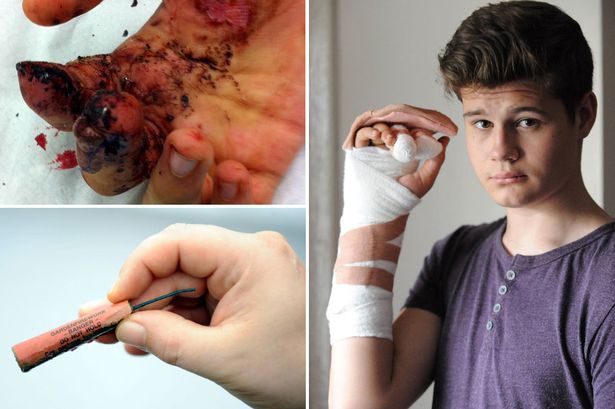
Fireworks and Kids: Who Wins In A Fight?
July 4th is upon us in ‘the states.’ The day with the largest concentrations of explosions and other pyrotechnics of any; and the day with the greatest numbers of burn and explosive related injuries of any other in our parts.
Many areas have illegalized certain classes of fireworks for safety reasons. Of late much of the new legislations Even sparklers cause numerous injuries to children, especially eyes and prohibitions have been related to the fires they cause in tinder-box July weather.
Fireworks and Explosive Injuries
Realizing that other countries also have celebrations with “flashy lights and booms” during the year, I thought it might be interesting to pass along a little information from a “test your knowledge” quiz that I took recently in a medical article.
The latest statistics I’ve found come from 2012 when the National Fire Protection Association said that 8,700 people were injured by fireworks in the US. Most of those injuries were to the extremities (55%) but another 33% were to the head! Of course, they also added that more fires are reported on Independence Day than on any other.
Blast Injury Categories
Us medical types like to label and categorize everything in order to begin studying them. It’s no surprise that there are four general categories of blast injuries, just as there are different categories of burns. Do you know what they are?
- Primary: Injuries due solely to the direct effect of blast overpressure on tissue.
- Secondary: Those caused by flying objects that strike people.
- Tertiary: Those caused by high-energy explosions that cause people to fly through the air and strike other objects.
- Quaternary: All other explosive related injuries not in the first three categories
It turns out that there is a great correlation to severity, and thus treatment, the higher you go up this ladder of description. It would be hard for me to describe something that causes a Tertiary or above injury as a “firework.”
The thing about firework injuries is that pretty much all of them would be considered “needless” (being considered discretionary entertainment); most of them, I suppose, “accidental”; at least some of them sheer stupid; but all of them painful and damaging.
Burn Treatment
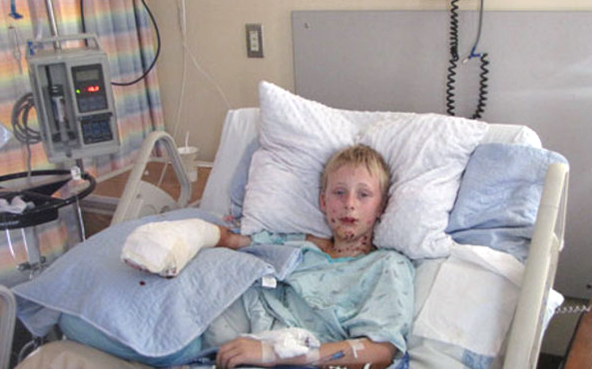
The injuries to children are, thankfully, mostly burns. I say thankfully only because as bad as burns can be, overcompression injuries are much, much worse and often permanent.
The article I’m describing told about four common treatments for burns (beyond first aid) which have been used. All but one are still being used today, can you guess which one isn’t? Topical antibiotics, Silver Sulfadiazine, topical steroids or popping and removing all big blisters (bullae).
Burns on the face and other such parts are best treated by means of an open technique; namely, washing the burn area, removing any open blisters and dead skin, and only covering the wounds with topical antibiotics and possibly a non-adherent, loose clean dressing. You want air exposure for the recovering tissues and don’t want anything sticking into the healing skin.
Fingers and toes are wrapped individually, with fluffed gauze separating the digits in order to prevent maceration and adherence.
All partial-thickness wounds are covered with antibiotic ointment. Silver sulfadiazine is commonly used but may not be available to the emergency physician. Steroids have no role in treating burn wounds. Cleanse other areas with minor burns using a mild soap and gentle scrubbing.
The World Health Organization (WHO) recommends debridement of all bullae and excision of all adherent necrotic tissue.
Burns and Fluid Resuscitation
As the size of a burn increases, it becomes important to consider how much fluid loss is caused – especially in children. Tissue damaged for any reason is disrupted to that point that it leaks fluid, sometimes directly out the wound but more often into the surrounding tissues. That’s what produces all the puffiness and swelling.
So much fluid can leak out of the cells so quickly that fluid is pulled out of the blood-stream. When that happens the whole body suffers the effects of dehydration. That is why pediatricians are extremely careful to start IVs and watch urine output.
There are even charts that we use to calculate how much fluids to replace; which, it seems lately, causes another problem. In the quiz that I took most physicians responded that insufficient hydration, not recognizing signs of cardiac failure and not using a pulmonary artery catheter were the most common errors of fluid resuscitation. In fact, only 26 percent of us knew that OVER-hydration was the correct answer for the most common error in treatment.
We now know that even though fluid resuscitation is critical, overdoing it can increase the risk for acute respiratory distress syndrome about 3-5 days after the burn. Especially for those children (and adults) with large total body surface area (TBSA) burns or who have inhalation injuries, these days we modify the standard formulas downward a little and follow catheterized urine output much more closely.
Use of Burn Centers
Needing to treat severe burns, again I say thankfully, is not common even though it is not uncommon. By that I mean they do occur often enough for us to have experience with them and have developed new “best practices” for treatment and repair; but, not frequently enough that EVERY doctor has very much experience or that EVERY hospital will have the right equipment or staff.
That’s why you’ve heard of “burn centers” – facilities equipped and staffed to receive transfers of patients who are most severely burned. They are great places and many studies have shown that patients who can be transferred to them stand a better chance at better recovery.
Even though each patient is individualized the American Burn Association has guidelines about which patients should and when they should be transferred:
Guidelines For Transfer of Burn Patients
- Any partial-thickness burn larger than 20% of TBSA in a patient of any age, or larger than 10% of TBSA in children younger than 10 years or adults older than 50 years
- Third-degree burns covering more than 5% of TBSA
- Second-degree or third-degree burns involving critical areas (eg, hands, feet, face, perineum, genitalia, or major joints)
- Burns with associated inhalation injury
- Electrical or lightning burns
- Severe burns complicated by coexisting trauma; if traumatic injuries pose a higher risk to the patient than the burn injuries, the patient may have to be sent first to a trauma center
- Preexisting disease that could complicate management of the burn injury
- Chemical burns with threat of cosmetic or functional compromise
- Circumferential burns on the extremities or the chest
Blast Injuries
Perhaps in an article about children’s fireworks and injuries I should stop here. However, I will continue on to at least mention “blast injuries” if only to point out that they are a completely different animal and just due to body size alone are escalated in severity in children.
Commonly in blast injuries not all damage to tissue is readily seen. Internal injuries and injuries with delayed observability are, unfortunately, the norm. Fortunately they occur only rarely but that means that we haven’t yet been able to develop definitive guidelines about them. We currently use the following thought processes:
Open-space explosions are greatly less damaging than in closed-spaces or in water where the damaging compressive waves impact more inward to the victims. Patients in open-space explosions who don’t have any apparent significant injury, have normal vital signs and normal physical exams can often be observed for 4 hours then discharged to home with instructions to come back if there is any shortness of breath, abdominal pain, vomiting or other symptoms.
If the explosion was closed-space or in water, or bad enough to rupture the ear-drum, there is much, much more risk of delayed complications. These patients get imaging studies of their chests and other organs along with intensive monitoring over a longer period. Rarely a highly motivated, reliable adult who is completely without symptoms might be sent home after 4 hours – children almost never are.
Complications are so common in some instances that even without currently observable clinical findings victims are admitted to the hospital. Such would be: significant burns, suspected air embolism, radiation or water pollution contamination, abnormal vital signs, abnormal lung examination findings, clinical or radiographic evidence of pulmonary contusion or pneumothorax, abdominal pain, vomiting, evidence of renal contusion/hypoxia, or penetrating injuries to the thorax, abdomen, neck, or cranial cavity.
[http://reference.medscape.com/viewarticle/847137]
Advertisement by Google
(sorry, only few pages have ads)