Treating Appendicitis Without Surgery May Work
I have to say that reading the research study that I’m commencing to tell you about kinda’ caught me a bit off guard and I’m still trying to “process” it. Treating proven appendicitis in children without surgery – who would even try it the first time to see if it would work?
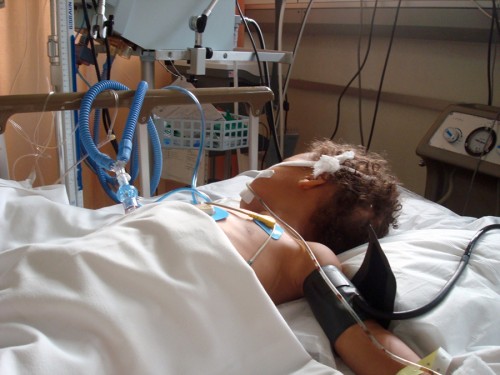
Child with ruptured appendix from appendicitis in the ICUI mean, this is one disease where nearly every pediatrician has had several cases in his very own practice and therefore has very strong memories. I had FOUR in my very first week of residency!
One was “signed off” to me by the outgoing resident, one my attending (meaning I did the work) was consulting to the surgeons in the ICU where he (the patient) was unconscious, one was admitted to my ward by the ER resident whose “guess” turned out to be correct and one that I saw in the clinic whose symptoms screamed appendicitis and nothing else, but… alas… wasn’t – so left the parents and all of us still wondering.
Appendicitis
Most of us have heard horror stories about the days before penicillin when patients out in the bush with appendicitis were packed in ice while everyone stood by and watched as they either survived… or not.
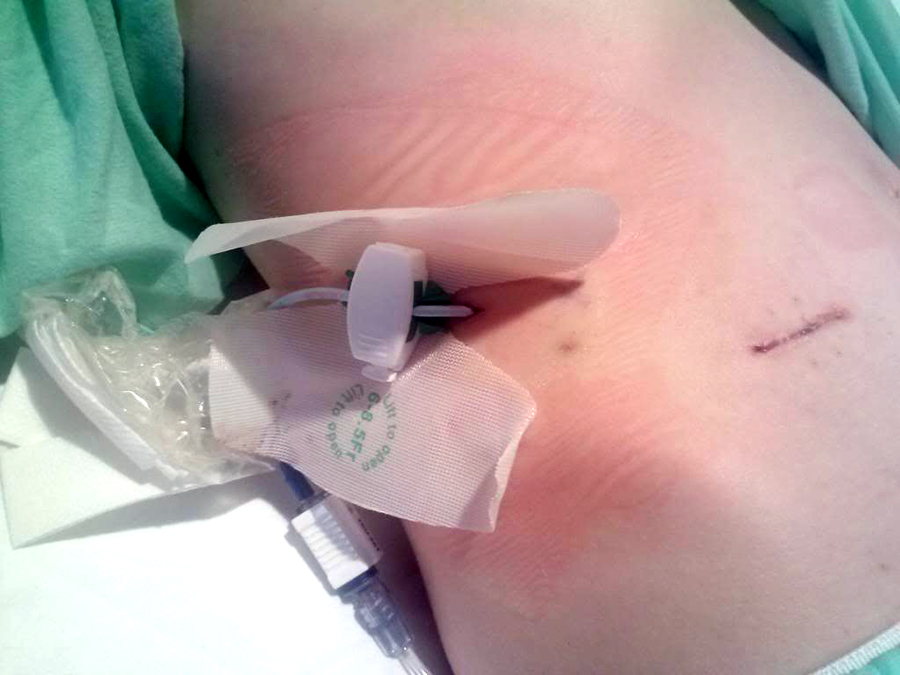 Ruptured appendicitis, drain of abscess, scar at McBurney’s pointIt’s the rupturing and spilling infection all over inside the belly that is the real horror us doc types have nightmares about. If that occurs a lot of other things begin spiraling downward to a possibly very unhappy ending.
Ruptured appendicitis, drain of abscess, scar at McBurney’s pointIt’s the rupturing and spilling infection all over inside the belly that is the real horror us doc types have nightmares about. If that occurs a lot of other things begin spiraling downward to a possibly very unhappy ending.
Fortunately, the little thing hanging out right where the big and little intestines meet was found to be perplexingly functionless and unnecessary, so surgeons could remove it any time they wanted (and could get at it) with impunity. In the case of appendicitis, hopefully before the beastly thing actually ruptured.
There have always been two or three caveats in our procedures. First, of course, is the fact that… it’s surgery. And who really wants to do that? Then there’s the fact that sometimes just the mere touching of the thing causes it to burst right there in surgery.
That’s why everyones preference has been to have the patient on fairly strong antibiotics for a fair while (if all the events will let us) before doing surgery. And, there’s that pesky occurrence when absolutely everything reveals a diagnosis of appendicitis BUT when it’s removed there is no inflammation there at all.
Treatment Without Surgery
Now days surgeons have gotten more skilled, antibiotics have gotten stronger, medical care more available, patients wiser about symptoms and even diagnosis more secure with all the imaging and sophisticated tests. In that setting is this new research about treating without doing surgery.
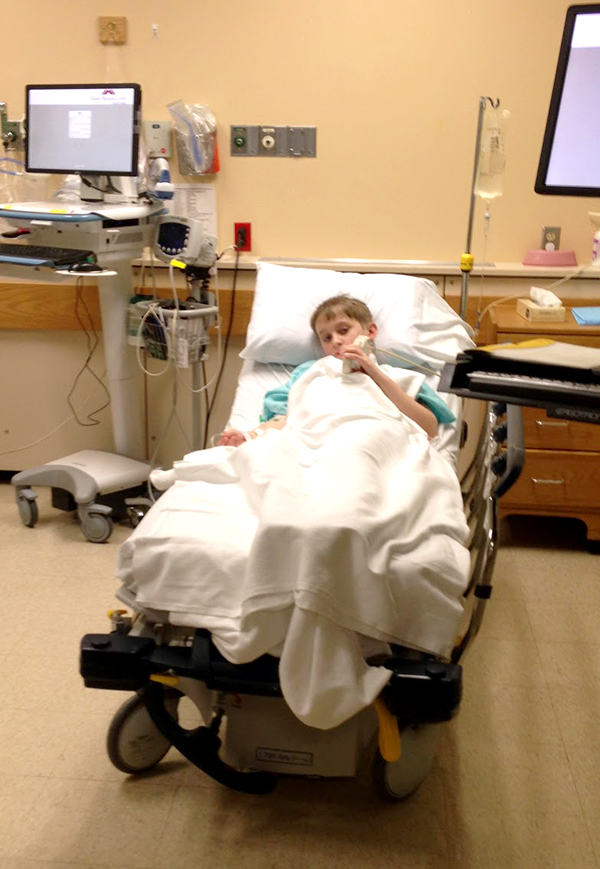 Boy with appendicitis receiving antibiotic in ERThe docs at Nationwide Children’s Hospital in Columbus Ohio compared surgical versus nonsurgical management of uncomplicated acute appendicitis in 77 children and reported about it in the Journal of the American College of Surgeons [Apr 12, 2014]. The “non-surgerized” children were hospitalized for observation and antibiotics for a minimum of 24 hours along with nothing to eat or drink for at least 12 hours.
Boy with appendicitis receiving antibiotic in ERThe docs at Nationwide Children’s Hospital in Columbus Ohio compared surgical versus nonsurgical management of uncomplicated acute appendicitis in 77 children and reported about it in the Journal of the American College of Surgeons [Apr 12, 2014]. The “non-surgerized” children were hospitalized for observation and antibiotics for a minimum of 24 hours along with nothing to eat or drink for at least 12 hours.
They were then switched to oral antibiotics, for a total 10-day course, as soon as they were tolerating a regular diet – and it worked! At least for 27 of the 30 children that they used it on, giving an immediate and 30-day success rate of 93 and 90 percent respectively.
However, only the very simplest and easiest of patients were treated that way – we call that “cherry-picking.” All patients 7 to 17 years of age with appendicitis between October 2012 and October 2013 were considered for the study.
If they hadn’t had pain for over 48 hours and if their CT or Ultrasound showed NON-ruptured appendix less than 1.1 centimeter in diameter without abcess or “liths” then they attempted treatment without surgery. As I’ve said 47 didn’t qualify and went to surgery – 30 did.
Then, of the 30 patients, 2 patients underwent laparoscopic appendectomy while they were in the hospital because they didn’t show sufficient improvement and one was re-admitted because the pain came back and also had a laparoscopic appendectomy.
Even though not all escaped surgery, close to half did and of course they returned to school sooner (3 vs 5 days), experienced fewer disability days (3 vs 17 days), and reported higher quality-of-life scores for the patient (93 vs 88), as well as the parent (96 vs 90). Not bad.
Really, when I look back at it, what’s the point of having a real “easy” case of appendicitis if you get the same treatment? This treatment alternative makes sense if you can catch it early in the course and the doctors further note that even among those three who tried to make it without surgery “there was no progression to rupture at the time of (their needed) appendectomy.” Pretty much a win-win!
The Rest Of The Story
Was there any down side? Well, the children without surgery stayed in the hospital a bit longer than those who had surgery (38 vs 20 hours) because they still required in-hospital monitoring for clinical changes that might warrant surgical intervention. However, their costs were a whole lot lower due to avoiding the exorbitant fees associated with surgery these days.
As a final shot the researchers stated that they pretty much expected a good result because it would be consistent with results in adults where non-operative management is currently the accepted initial therapy in many European hospitals. They also say that they are now beginning a 1-year follow-up evaluation of the safety, success rate, and cost-effectiveness of the non-surgical approach to uncomplicated appendicitis in children.
[J Am Coll Surg. Published online April 12, 2014. Abstract]
Advertisement by Google
(sorry, only few pages have ads)