Summer Childhood Illnesses and Injuries – Part 2
The injuries and illnesses parents must worry about their children getting into changes direction once the crocus blooms and the snow melts revealing a whole new set of things to worry about.
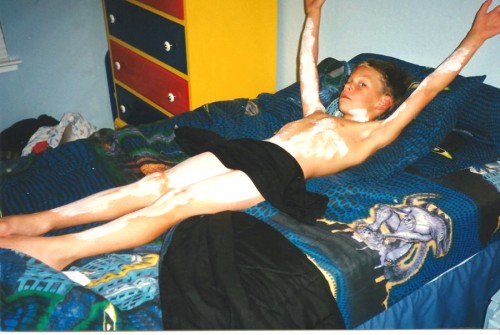
The Emergency Room’s start filling up with children suffering12 year old boy treated for Rhus Dermatitis – Poison Oak issues not often seen during winter, and those are the things we’re talking about in these two articles: Summer Childhood Illnesses and Injuries.
Even including part one of this series where we talked about submersion injuries, diving injuries, heat injuries, concussions and external ear infections, this obviously isn’t a complete list of all children’s summertime problems – that would take a book – nor is it comprehensive for each issue.
It does, however, serve as a “memory jog” that parent’s can use to “switch gears” from their winter worries to those needed in the summer. We’ll continue by talking about: the dreaded rashes.
Summertime Things to Watch For and Prevent
Summer rashes tend to switch from those which are a site-effect of viral rashes (contracted through contagion) to those inflicted by some activity.
Rhus Dermatitis
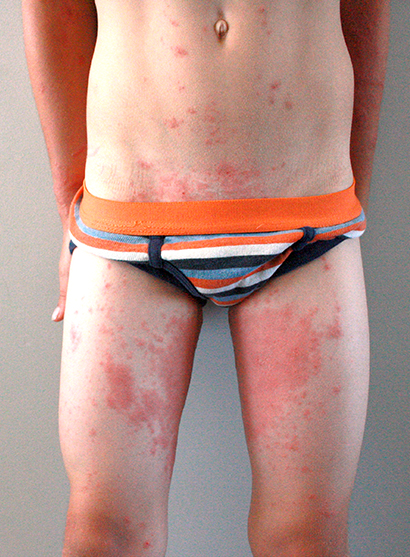 Boy with Poison Ivy rash in usual placesProbably the first thing every boy scout learns in first aid is the dreaded: Poison Ivy – how to recognize it, avoid it and wash with soap and water “from the outside inward” in order not to spread it all over to other skin.
Boy with Poison Ivy rash in usual placesProbably the first thing every boy scout learns in first aid is the dreaded: Poison Ivy – how to recognize it, avoid it and wash with soap and water “from the outside inward” in order not to spread it all over to other skin.
It’s not just the ivy that is poison but there’s also poison oak and poison sumac (all from the genus Toxicodendron) which produce the “rhus” antigen that can cause the often linear, erythematous (red), edematous (puffy) and terribly pruritic (itchy) rash known as Rhus Dermatitis – and we’ve written about it before.
About 10-15 percent of the population have extreme sensitivity to the Rhus antigen, which then leads to generalized reactions in addition to the local sensitivity. Older children sometimes can report a known exposure but many are afflicted unknowingly during play or even by pets who have been in the plant.
A RE-sensitization can occur by contacting clothing or linens which have been contaminated and the most severe reactions come from inhaling and contacting smoke from burning plants.
TREATMENT: Washing with copious water and soap (outside in, wearing gloves) within 20 minutes of exposure helps. Also topical preparations such as: Domeboro®, calamine, oatmeal baths and Burow solution are used. Oral antihistamines help itching and steroids are used in severe cases.
Sunburn
Getting a first degree burn (outer layer of skin) from sun exposure is almost a “rite of passage” for most children. Once old enough that they can be enough of a moving target to escape parental radar, about half of the population of children get a sunburn every summer.
Ultraviolet radiation from any source – tanning beds, phototherapy lamps or the sun – can burn the skin in unexpectedly short time. By the time you feel the burn, it’s way too late.
The inflammatory response which peaks in about 12-24 hours can result in edema and blistering, especially in the fair-skinned, blue-eyed and blond or red-headed.
TREATMENT: Stopping continued heat exposure is critical. Cool baths help – but not long enough to “wrinkle” and damage the skin further. Cool compresses and emollients are standard treatment – especially Aloe Vera. Topical analgesic creams such as Nupercainal, can help in severe cases.
Children whose burns are more extensive in size or are second degree (deeper) often require much more substantial therapy with fluid resuscitation.
Insect Bites and Stings
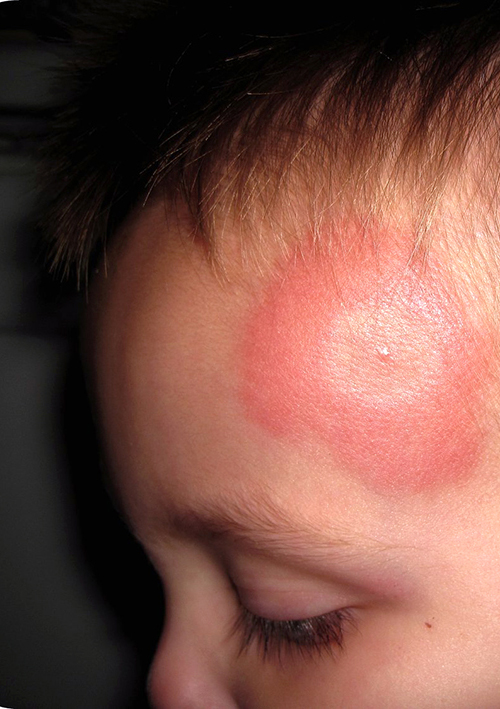 Boy with spider bite on foreheadIt’s annoying when we doctors ask questions like: “Is it a bite or a sting” isn’t it? But, in this case it matters.
Boy with spider bite on foreheadIt’s annoying when we doctors ask questions like: “Is it a bite or a sting” isn’t it? But, in this case it matters.
A BITE is merely the result of you becoming a food source for an insect (mosquitoes, fleas, mites, bedbugs etc.) during it’s normal course of feeding. A STING, on the other hand, is an aggressive action of an insect (bee, hornet, wasp, scorpion etc.) to penetrate you with a venom. One merely itches, the other causes local tissue damage and/or effects on bodily organ systems.
Additionally, in either case, one’s own body can add to the misery by reacting with sensitivity and a systemic reaction ranging from mild to fatal.
Because both insects and their food sources are active in the summer, that’s when bites and stings peak.
Within minutes a local reaction of wheals and urticaria appear with itching, pain, redness, soreness, warmth and swelling. If the reaction is particularly strong with redness, welts and swelling then a systemic reaction is likely with a subsequent exposure.
Generalized anaphylaxis can begin with rash and symptoms not even local to the bite, then rapidly progress to disorientation, fainting, anxiety, hypotension and vascular collapse or death. Or, it may wait for up to two weeks to produce symptoms of serum sickness.
TREATMENT: is with routine wound cleansing then ice for most occurrences. Systemic reactions are treated with injectable Epinephrine even prior to going to the Emergency Room.
Wounds
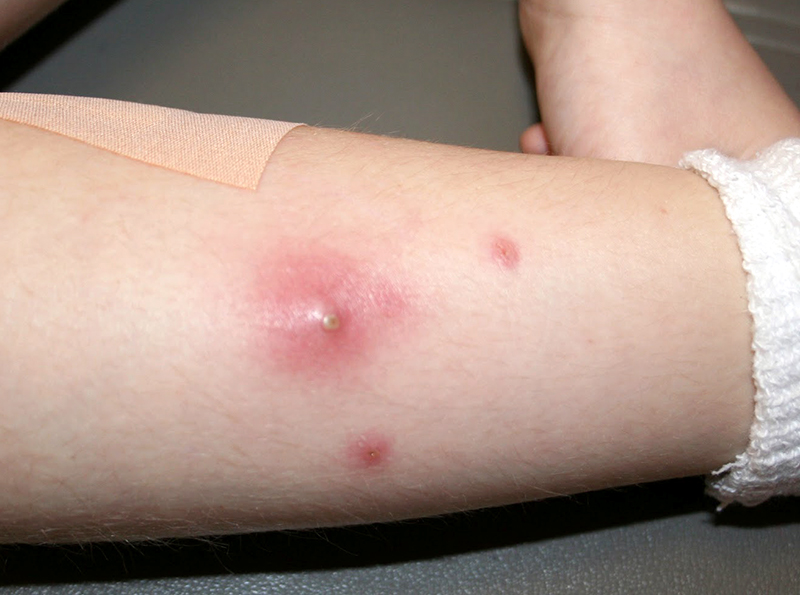 Wounds need to be on this list because they definitely increase in number during the summer months. But, where to begin? There are so many different types. Bangs, bruises, cuts and abrasions, burns and blisters are all… like, a mandatory part of summer for children.
Wounds need to be on this list because they definitely increase in number during the summer months. But, where to begin? There are so many different types. Bangs, bruises, cuts and abrasions, burns and blisters are all… like, a mandatory part of summer for children.
What they all have in common these days, however, is the possibility of becoming infected with Methicillin Resistant Staphylococcus Aureus (MRSA) the “community acquired type.” Meaning the type of bacteria for which we have NO antibiotic’s that can kill it!
For doctors, it’s almost like being back to the “dark ages” (ie before antibiotics) and we’re back tap-dancing on thin ice trying to identify “best methods” of how to handle them in order to avoid significant morbidity – amputation or death is never good.
The latest guidelines require physicians to individualize therapy according to clinical symptoms and local area “antibiograms” (patterns of resistance). Methods are different depending upon whether it’s purulent (pus forming) or non-purulent as well as whether it is Mild, Moderate or Severe.
Treatment of purulent cases (abscesses, furuncles and carbuncles) are often addressed with incision and drainage, without antibiotics unless there are systemic symptoms such as fever. Infected non-purulent wounds have nothing to drain and are more frequently treated with what antibiotics we do have.
Severe non-purulent cases are debrided surgically (cut away) based on physician judgment using physical diagnosis, clinical course and information about local organisms.
Lawnmower Injuries
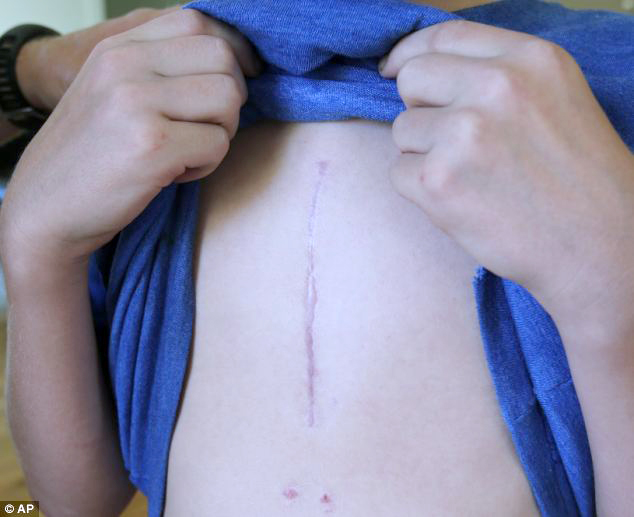 Boy showing scar from nail thrown into his heart by a lawnmowerThe first time I started up the lawnmower this summer it threw a screw which had fallen off the deck clear across the patio and stuck it in the siding of the house!
Boy showing scar from nail thrown into his heart by a lawnmowerThe first time I started up the lawnmower this summer it threw a screw which had fallen off the deck clear across the patio and stuck it in the siding of the house!
What a wake-up call that summer vigilance was upon us! What if that had been the neighbor kid that we hire to mow the lawn?
We’ve posted about lawnmower injuries previously but this issue must be included in any post about summertime dangers in childhood.
By no means is the only danger those blades whirling around. Any power mower will suck up rocks, glass, nails, screws and any shards of metal right out of their hiding places deep in the grass and throw them with enough force to do mortal damage to a child many yards away.
There is NO safe place to stand and watch grandpa mow the lawn except behind some protective shield.
Food-borne Illness
It really wouldn’t be right to get you worrying over your kids about summertime activities and completely leave out all the picnics and Food-borne Diseases (FBDs)!
We are WAY above the Healthy People 2020 targets that we set in the U.S. for FBDs, especially among children under 5 years old. There are several bacterial causes, Salmonella being the most common and accounts for the most hospitalizations and deaths these days in this country.
Children are prone to the hemolytic-uremic syndrome as a sequelae to the E Coli produced bloody diarrhea; but staphylococcal-toxin and Vibrio Cholerae also produce diarrhea and are found in spoiled or contaminated food.
Determining how long it took for symptoms to occur after ingestion of the contaminated food is important in identifying the cause and possible treatment.
Do NOT eat food that hasn’t been kept cold and iced – especially those milk, butter, mayo based.
Treatment is largely supportive with fluids and electrolytes, antibiotics are usually not warranted.
2 Posts in Summer Illnesses (summerillnesses) Series
- Summer Illnesses 2: Poison Ivy - Food Poisoning – 14 Aug 2014
- Summer Illnesses 1: Drowning-Otitis – 2 Aug 2014
Advertisement by Google
(sorry, only few pages have ads)