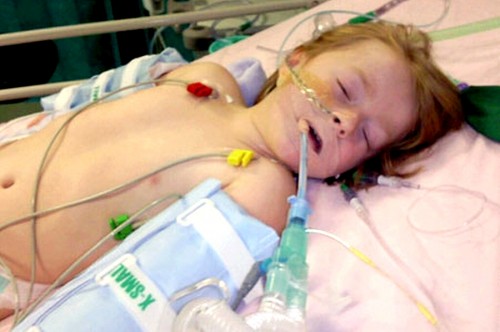
Most Severe Influenza: Young, Unvaccinated Adults
This is one of those instances where the title of the article almost tells you its whole content: Influenza isn’t just an “old people’s disease” anymore. And, being young and otherwise vigorous doesn’t keep you from ending up in the intensive care unit and possibly dying!
Lets take some up-to-date examples of what’s happening this (2014) flu season. One of the first institutions to let the world know what it’s experiencing is Duke University Medical Center in Durham, North Carolina.
Influenza In The 2014 Season
- It only took them from Nov 2013 to Jan 8, 2014 to have 22 patients admitted to their Intensive Care Unit for Influenza.
- Of those admitted to the ICU, only 2 had been vaccinated before their illness – 91% of ICU Influenza admissions had NOT been vaccinated.
- In that period, of the first 55 patients seen, 48 were infected with the H1N1 virus (87%) – similar to the 2009 epidemic which also was particularly severe in young adults.
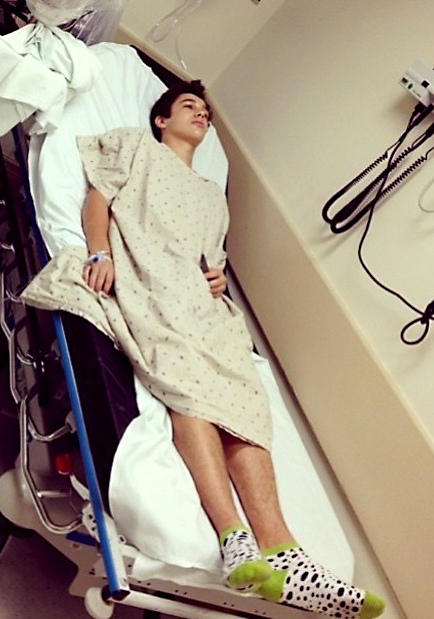
- Most hospitalizations were in previously healthy young persons, with a median age of 28.5 years (range, 2 months to 101 years).
- Young adults who had not been vaccinated against influenza had severe cases and needed the most intensive treatment.
- Of the remaining 33 patients who were admitted to the hospital, but didn’t need the ICU, only 11 (33%) had been immunized. Most of these patients were immunocompromised or immunosuppressed as a result of medication or were chronically ill.
- Overall, less than a fourth (23.6%; 13/55) of patients admitted to the hospital had been vaccinated against influenza at least 2 weeks before the onset of their acute illness.
 Let’s keep in mind that a vaccination costs less than $30 in the US and is readily available – almost on every street corner. [From a business standpoint, we see that there must be a good enough profit margin in it such that nearly every supermarket pharmacy and even box-stores are jumping into the market.]
Let’s keep in mind that a vaccination costs less than $30 in the US and is readily available – almost on every street corner. [From a business standpoint, we see that there must be a good enough profit margin in it such that nearly every supermarket pharmacy and even box-stores are jumping into the market.]
Problem With “Rapid Test”
One of the problems the doctors at Duke reported noticing while they were compiling these statistics was that 32% of those patients admitted to the ICU had seen a physician previously and had a previously negative influenza test.
We know that there are some false negatives when using the “rapid test” for influenza (patients with the disease NOT showing up on the test); but, this makes it difficult for a physician to rely on their results when deciding on whether or not to begin treatment with Oseltamivir, a very expensive medication.
The conundrum is that the medicine is not only expensive but that it doesn’t cure the disease, only shorten its duration and possibly severity, AND it only does that IF it’s begun within 24-48 hours of the onset of the disease.
In practice, that barely gives a stricken patient time to be seen by their doctor – even if they are able to strong-arm their way past the office triage and into an urgent appointment.
The answer, of course is that a physician should use the best judgment he can, taking into consideration each patients current condition, past medical history and current community levels of influenza. If a patient has “risk factors” for a more severe, complicated or progressive illness then treatment with antiviral’s should not await laboratory confirmation.
We don’t fault them, for it’s the way most clinician researchers talk; but, in their understated way, the Duke doctors who reported their findings merely state: “Added to the finding of very low vaccination rates among both hospitalized and ICU admissions, our observations support previous findings that vaccination reduces the severity of disease and vaccinations should be encouraged as recommended by the…Centers for Disease Control and Prevention.”
Ya think?!
[Am J Respir Crit Care Med. Published online February 10, 2014.]
Advertisement by Google
(sorry, only few pages have ads)