New Kids Health Guidelines In 2014
Today we go from previous posts on “Vintage Medical Advice” to several new treatment guidelines so “hot off the press” they are still smoking!
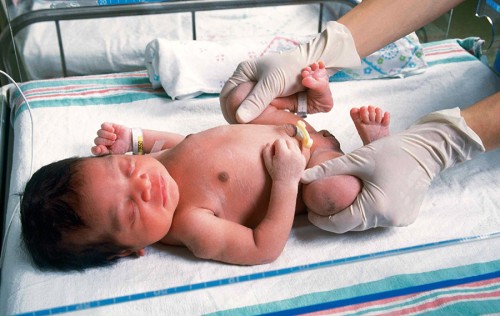
Ortolani Maneuver testing for dislocated hip in newborn
Medical research today is “night and day” different than what was done at the turn of the 20th century. Today, these guidelines are not just “consensus based” – a compilation of top doctors opinions but are “evidence based”, meaning that each aspect is formed from direct evidence found in meticulous research and usually verified through replication.
I think you’ll see what I mean as we go through the eight new sets of medical guidelines for the treatment of children which were published in 2014 — Congenital Hip Displasia (CHD), Calcium supplementation, Fluoride use, Respiratory Syncytial Virus (RSV), Drug testing, Anterior Cruciate Ligament (ACL) tears, Influenza and Autism.
Congenital Hip Dysplasia – Dislocated Hip
Congenital Hip Dysplasia, known as CHD for short, is a condition where an infant is born with more than the usual amount of laxity of the support structures in the hip. It’s not uncommon, which is why a good pediatrician does a thorough hip exam nearly every time they see an infant for the first year or so.
The problem comes due to the necessity of the body to have the leg bone (femur) nestled snugly into the hip socket in order to make the bones grow correctly around it. If they don’t, the hip will continually slip out of joint. The problem arises due to the fact that ALL babies have at least some laxity for several weeks after birth. How much is too much? And, if you think it’s too much, how do you diagnose it?
The American Academy of Orthopedic Surgeons reviewed the volumes of accumulated research and published the following guidelines for physicians to use in the diagnosis of the condition.
- Evidence shows we DON’T need to use ultrasound to screen ALL newborns for CHD as some thought previously
- Evidence shows we SHOULD do an imaging study on infants, before 6 months of age if we can, who have: breech birth, a family history of hip dysplasia or clinical instability on several physical examinations.
- And, some evidence shows that we should use simple pelvis x-rays rather than ultrasound to asses dysplasia if needed beginning at 4 months of age.
[ http://www.aaos.org/research/guidelines/DDHGuidelineFINAL.pdf ]
Calcium Intake and Supplementation
The American Academy of Pediatrics, the largest and most “official” organization for children’s medicine, reviewed the entire world’s research on calcium and bone health in children and published the most up-to-date information in an extensive set of standards and guidelines.
Although the developed world sees much less bone disease in children, what we consider simple diseases like Rickets are still major concerns afflicting the worlds children.
- The recommended daily allowance (RDA) of calcium for infants through 6 months of age is 200 milligrams per day then increases to 260 mg per day to 12 months.
- Calcium requirements (RDA) increase to 700 mg/day from 1 to 3 years of age, 1000 mg/day in 4 to 8 year olds and 1300 mg/day from 9 to 18 years.
- Extra supplementation of calcium in otherwise healthy children is unlikely to give a significant reduction in fracture risk.
Vitamin D is an essential vitamin required to absorb calcium. If it is inadequate in the body, only 10-15% of calcium in the diet is absorbed.
- From birth to 1 year of age, 400 International Units (IU) of vitamin D needs to be ingested daily. That rises to 600 IU through adolescence.
- Mothers who breast-feed should take 6000 IU of Vitamin D supplements daily otherwise their infants should receive Vit-D supplementation.
- Infants who are breast-fed, fully or partially, should receive 400 IU Vit-D supplementation from birth until they are weaned and drinking at least 1 liter per day of formula or milk fortified with Vit-D.
- Children older than 1 year who are: obese, receiving anticonvulsants, glucocorticoids, antifungals or antiretrovirals may require 2-4 times more than the 600 IU vitamin per day.
- Evidence does NOT suggest the need to screen ALL children for adequate Vit-D only children and teens who have recurrent low-impact fractures or who have conditions associated with reduced bone mass.
Researchers have invented several very sophisticated (and expensive) machines to measure bone density which have been tried in order to find out if they add anything to the doctor’s ability to diagnose and/or treat children. Additionally, some medicines have been tried to see if they will push bones to be stronger in many diseases; of course, not without side-effects.
- The use of dual-energy x-ray absorptiometry (a type of bone density test) should be considered only in children with medical conditions known to be associated with reduced bone mass or who have clinically significant fractures after only minimal trauma.
- Measurements with dual-energy x-ray absorptiometry should be considered for a teenage female who has been amenorrheic (absent menstrual periods) for greater than 6 months; OR, who fits the “female athlete triad” of low energy availability, menstrual dysfunction and reduced bone mass density.
- Evidence does NOT support the use of oral contraceptives to increase bone mass in those with either anorexia nervosa or the female athlete triad.
- Treatment with bisphosphonates should be restricted to children with osteogenesis imperfecta and conditions associated with recurrent fractures, severe pain or vertebral collapse.
[ American Academy of Pediatrics, September 2014]
Fluoride Supplementation
Fluoride is important for the development of strong teeth in children and prevention of cavities. It is a common mineral on the earth and is often found in water; but not in a uniform quantity. Many areas have too little in their water. A few others too much.
We’ve used fluoride drops and cities have added it to their water systems. Dentists have treated teeth with it and you can purchase toothpaste which is fluoridated. It’s the unintentional overdose of toothpaste in children which prompted the American Academy of Pediatrics to review fluoride guidelines last year (2014).
- Parents should use fluoridated toothpaste (although tiny amounts) for all children starting at tooth eruption.
- Parents should both dispense toothpaste and supervise/assist with brushing to assure that excess amounts are not swallowed or choked upon.
- Below age three only dispense a tiny smear of toothpaste, the size of a grain of rice.
- After age three a pea-sized amount may be used.
- Fluoride varnish is recommended in the primary care setting every 3.6 months, starting at tooth emergence.
- Over-the-counter fluoride rinse is not recommended for children younger than 6 years of age due to the risk of swallowing higher than the recommended amounts of fluoride.
[ Pediatrics. August 2014. http://pediatrics.aappublications.org/content/early/2014/08/19/peds.2014-1699.full.pdf]
Perhaps that’s enough to assimilate in one sitting. I’ll continue on with the remaining five new sets of children’s healthcare guidelines in the next article.
4 Posts in 2014 Medical Guidelines (2014guidelines) Series
- ACL Tears, Flu Vaccination and Autism – 15 Feb 2015
- RSV, Drug Testing – 7 Feb 2015
- Dislocated Hips, Calcium and Flouride – 3 Feb 2015
- 2014 Medical Guidelines: Intro/Index – 2 Feb 2015