Childhood Diabetes and a New Medicine – Part 2
Over 20 years ago, while I was in the service, a new method of testing diabetics for blood glucose control was “discovered” and I instantly seemed to know in my gut that it would revolutionize the care for the whole clinic full of patients I was managing – not to mention those kids at camp UTADA diabetic camp I saw every fall.Campers at Camp UTADA
So much so, that I applied for, and was awarded, a grant to study the use of “glycosylated hemoglobin” (GH or A1C) as a measurement of “control” in Juvenile Onset Diabetes Mellitus.
And, as I predicted, it literally HAS changed diabetic care for every diabetic in the world and even jump-kicked medical care onto a completely different track than it was on back then by setting complete “normo-glycemia” as the optimal goal; something that wasn’t considered because it was completely absurd back then.
Our only “standard” of measurement – the urine specimen – we now realize was pretty much totally worthless (like most of us thought) but blood measurements were only available in laboratories. It was largely the A1C values, which “tattled” about how effective a patient’s overall blood sugar control had been for the past several months, that taught us just how worthless urine sugar measurements really were.
It was also then that we had evidence that patients who got the bad complications of the disease were the one’s who had the higher A1C levels therefore the “worse” sugar control. All of this spawned new inventions, new innovations and new methods of care – synthetic insulin, home glucose monitors, insulin pumps and continuous glucose monitors.
Now my gut is “acting up” again when I read all the research articles coming out about the new discoveries in human “glucose control” that make up the “fine tuning” regulation the normal body uses. The single, “blood-sugar↭insulin” mechanism we’ve always known, just seems too simple to be all the normal human body uses – and it is… way is!
“New” Treatment For Childhood Diabetes
Injectable Glucagon-like Peptide-1 (GLP-1)
 Camps for diabetic children exist in every US stateIn the previous article we went through the discovery of insulin and even glucagon which have to date saved the lives of countless people with diabetes. And, we touched on the newly discovered “glucagon-like” compounds made by the gut which help in the “fine control” of the blood’s sugar level.
Camps for diabetic children exist in every US stateIn the previous article we went through the discovery of insulin and even glucagon which have to date saved the lives of countless people with diabetes. And, we touched on the newly discovered “glucagon-like” compounds made by the gut which help in the “fine control” of the blood’s sugar level.
The new development that has spawned my pontification here is that the injectable glucagon-like peptide-1 (GLP-1) agonist liraglutide (Victoza, Novo Nordisk) has now been shown to be able to benefit patients with type 1 (juvenile) diabetes when used right along with their insulin at least as well as it does those with type 2 (adult) diabetes.
Ok, the study was sponsored by Nordisk one of the manufacturers, but the good docs in Buffalo NY who did the 12-week randomized trial have now shown that A not-insignificant number of children will be able to obtain a HbA1c level of 7% or below without too much additional hypoglycemia – in addition to weight loss and blood-pressure benefits, a huge, huge benefit.
The fact that only using diet and insulin (even with pumps) is at best only “gross control” still leaves about 40% of those with type 1 diabetes to develop “metabolic syndrome,” a constellation of problems associated with obesity. These “glucagon-like” drugs seem to be able to use their fine-control “magic” to target three of the syndrome’s five features: high blood pressure, diabetes, and obesity.
Until now, the necessary studies to show effectiveness in type 1 diabetes were put on the back burner in order to enable FDA approval in the largest market, adults. But now, this study is a first step to gain approval in perhaps the most “meaningful” market – i.e. the youngest who will have the disease the longest, especially if this works like we think it will.
Using it adds yet another injection, because it’s only currently available in that form, and because it’s not yet FDA approved it is considered “experimental” under most health insurance and not covered; however, if the results of this study can be verified, there is: less hypoglycemia, 25% less insulin use, a drop in BP, a drop in excess weight and a reduction in glycemic variation.
Type 1, GLP-1 Study
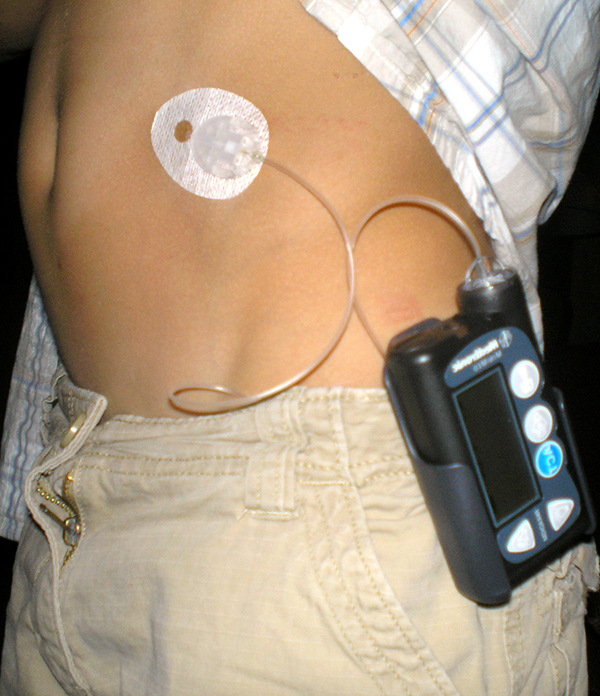 Boy with diabetes wearing an insulin pumpWhat, to me at least, seems like a great way to have done it, the researchers took 72 type 1 diabetes patients, all who were using both insulin pumps and continuous glucose monitors, and randomized them to one of three doses of GLP-1 or placebo. The group, as a whole, averaged an age of 44, duration of 24 years, overweight, high BMI and a mean A1C of 7.5%.
Boy with diabetes wearing an insulin pumpWhat, to me at least, seems like a great way to have done it, the researchers took 72 type 1 diabetes patients, all who were using both insulin pumps and continuous glucose monitors, and randomized them to one of three doses of GLP-1 or placebo. The group, as a whole, averaged an age of 44, duration of 24 years, overweight, high BMI and a mean A1C of 7.5%.
Ok, they weren’t what we were consider “kids” like I would have liked; but, 63 (88%) made it all the way through to 12 weeks and they did use a “placebo” group to compare and none of them knew which medicine they were getting. And, they could have made it better by running everyone through again with the “alternate” group, but that doesn’t diminish what they actually DID find.
Mean blood glucose levels had dropped by about 10 mg/dl and A1C dropped by 0.8% (great for only being 3 months); both of which were statistically significant over the placebo group. As one would expect, the patients farther out of “control” had the most benefit in their A1C levels. Those starting with lower A1C levels had the biggest drop in their insulin amounts.
The two higher dose groups (of GLP-1) spent more of their time in the “normal” sugar range and less in the “higher” range according to their continuous monitors. There were no severe “low” sugar events but the two higher dose groups had about 1% more time in the “low” range – the low dose group matched the placebo group.
Required insulin dose dropped by 10-12 units in the two higher dose groups – statistically significant; and, body weight dropped significantly in all three groups (5kg in two higher dose groups and 3kg in the lower dose group) when compared with the placebo group. This led an investigator to write “these people had a remarkable weight loss.”
Why is weight important? Well, diabetics have the same problem as the rest of us: if your exercise doesn’t match the food intake (and insulin) you get fat! And fat makes almost everything, everywhere harder especially diabetes management and side-effects.
 Obese boy with type 2 diabetesEven the few patients of normal weight in this study showed benefits of the drug: A1C dropped 1-0.5 percentage points with a 10% reduced insulin requirement.
Obese boy with type 2 diabetesEven the few patients of normal weight in this study showed benefits of the drug: A1C dropped 1-0.5 percentage points with a 10% reduced insulin requirement.
And the entire group of patients dropped their blood pressure by up to 9mm Hg – even the low dose group dropped by 5mm Hg when they didn’t seem to benefit in blood sugar levels. You see, the effects of GLP-1 on glycemia, weight and blood sugar are independent of each other.
What’s To Come?
Unless my gut is wrong, this is just the beginning of another lunge forward in diabetes care and management.
The other manufacturers of GLP-1 drugs are already conducting similar trials we will read about in the weeks to come as they try to expand their label indications to include type-1 diabetes.
Companies are doing the same for DPP-4 and SGLT-2 inhibitor drugs as well; and, unless I miss my guess there will be studies that show the benefit for GLP-1 in Type-2 diabetes as a “first-line” drug (i.e. without insulin) perhaps with existing oral medications.
I promised the kids in my cabin at camp that someday medicines will be easy and bring “control” back to normal – 25 years ago I didn’t have the temerity to get their hopes up for a cure. But, who really knows?
[American Association of Clinical Endocrinologists 23rd Annual Scientific and Clinical Congress. Presented May 16, 2014]
2 Posts in Childhood Diabetes (diabetesmed) Series
- Part 2 - GLP-1 Meds – 27 Jun 2014
- Part 1 - Diabetes history, GLP-1 – 23 Jun 2014

