BMI Not Correlating With Activity Level in Children
Finally, after years and years of badgering and nay-saying by pediatricians, politicians and others are awakening to the national dilemma that is: our kids are becoming WAY, WAY too fat! Not the most politically correct way to say it; but, there you are.
Childhood obesity epidemic, is BMI a good measure
The time for mincing words and beating around the bush is over. BUT, just like in other crises, there’s a lot of “stupid” going on. Politico’s are “illegalizing” large size soft drinks, airlines are scamming passengers by the pound and children’s organizations are setting restrictions based on BMI calculations.
A recent study merely explains what physicians have been taught in medical school for at least 25 years that I know of: “BMI measurement is a good and valuable ratio of height and weight in everyone but does NOT necessarily equate to either obesity or a healthy body condition” – because, there is more contained in the body that “weighs” other than fat.
Of Course BMI Doesn’t Necessarily Mean Obese
Basic Metabolic Index (BMI)
The best I can tell, the term “Basic Metabolic Index” was coined by some administrator somewhere trying to aggrandize already available height and weight charts into a new “catchy” name that he could take credit for.
It has only the most indirect relation to the term “metabolic” and is only vaguely an “index” – unless you count “divide weight by height” an “index.” Most of all, while actually being minimally useful it can be terribly misleading.
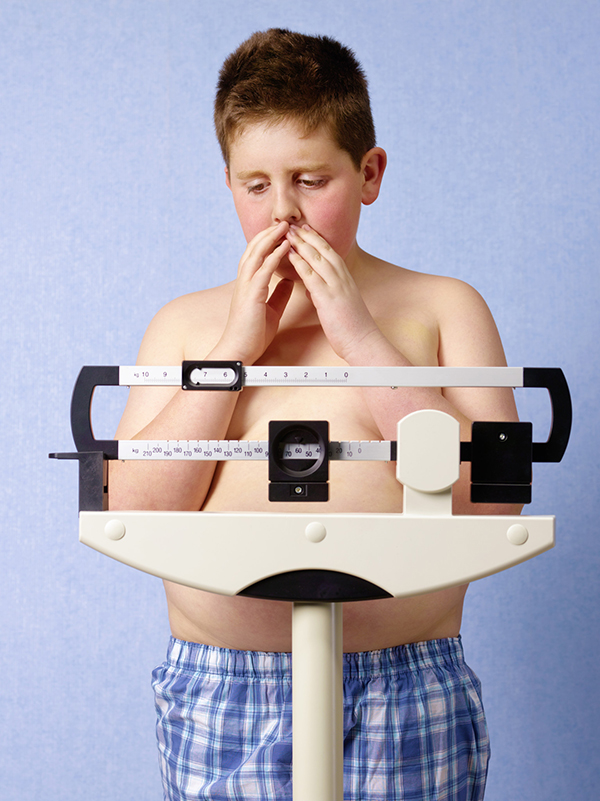 Childhood obesity has reached epidemic proportions in the USThe tried and tested “growth charts” utilized by children’s health researchers and pediatricians all over the world acknowledge a wide variation in what is considered “normal”; so, indicate wide ranges of “percentiles” which need to be printed separately for “boys and girls” as well as for other considerations such as genetic syndromes and even race. The BMI calculations tend to minimize the variability in its math.
Childhood obesity has reached epidemic proportions in the USThe tried and tested “growth charts” utilized by children’s health researchers and pediatricians all over the world acknowledge a wide variation in what is considered “normal”; so, indicate wide ranges of “percentiles” which need to be printed separately for “boys and girls” as well as for other considerations such as genetic syndromes and even race. The BMI calculations tend to minimize the variability in its math.
Which is why two completely different children can have the exact same BMI and one be obese while the other is “normal.” At any given age and gender a child’s weight can be made up of bone, muscle or fat – in any proportion. Too much fat is considered obese; but, exchange an equivalent weight of fat for muscle – AND THE BMI REMAINS THE SAME! It’s merely math, after all.
Exercise and BMI
So, if you can’t reliably count on a persons BMI measurement to accurately depict obesity, what about exercise? Does the BMI predict more “active” and “sports minded” children from those more sedentary and “couch oriented”? Sorry, no!
Researchers using the massive “twins registry database” of the Netherlands reported on their recent study which showed no strong correlation with that either. Since 1987, over 10,500 sets of twins have been followed in the country and the researchers contacted those 7 – 18 years old to obtain estimates of their weekly energy expenditures – “weekly metabolic equivalents of task.”
Then, they used the best standardized BMI calculations and compared activity levels – surprise, the very lowest activity level children were found in both the lowest and highest BMI quintiles (portions).
“Not only that,” they reported to this year’s sports medicine meeting in Florida, “those who had an increase in BMI did not necessarily become less active, and subjects whose BMI decreased did not become more active.” And, the same findings have been seen in other large studies for both adults and children.
Exercise – it clearly has massive health benefits and is an integral component for controlling weight; but, its benefits are much more obvious and measureable in health and well being than it is in BMI. Positive changes in blood chemistry, for example, can be seen within weeks of changing exercise life-styles.
What Does This Mean?
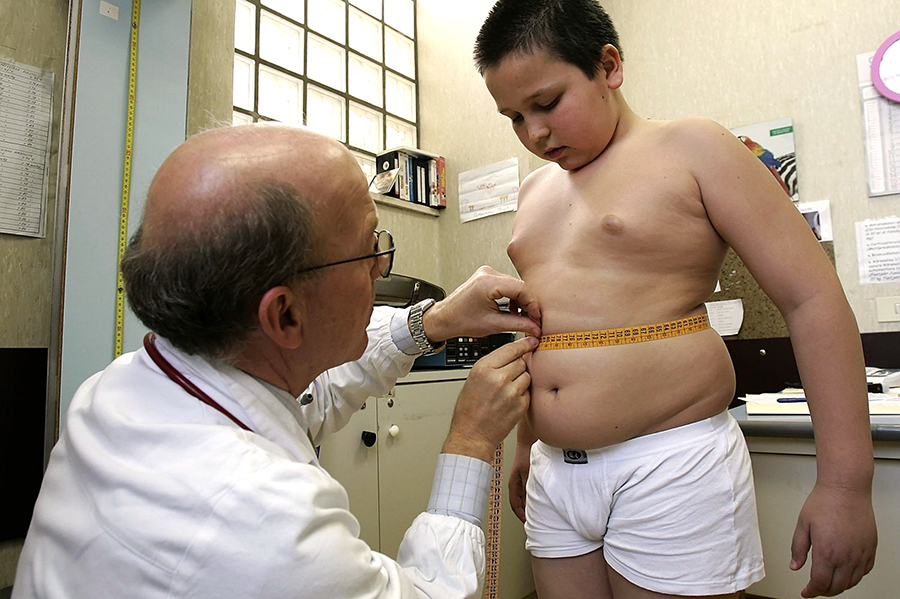 There is no substitute for a good physical exam by a pediatricianWhat, then, does this mean? First of all, the definition of obesity is clearly more complex than simply calculating the BMI – no matter what standardization one uses.
There is no substitute for a good physical exam by a pediatricianWhat, then, does this mean? First of all, the definition of obesity is clearly more complex than simply calculating the BMI – no matter what standardization one uses.
Being “big boned” or “all muscle” can still be a “cop out” and excuse for being over weight; but, the BMI calculation is merely ONE TOOL that a physician should use. Actually, a pediatrician RARELY even needs to calculate it – except to put on physical exam forms – because he has an even more accurate assessment tool… merely “look” at the child during the physical exam.
Thousands of exam’s worth of experience in looking at children of all sorts and sizes gives the expertise; AND, the good news is that more of us are actually getting up the nerve to mention excessive weight to parents.
It would be great if we really had an objective measurement that correlated with a person’s activity level, we don’t yet. Who knows why not all people who exercise lower BMI? Perhaps they compensate by increasing calorie intake or simply gain muscle mass or even start to drop exercise in other areas (like taking elevators and cars).
Perhaps one day we’ll have a quantifiable indicator of exercise to study obesity like we now have the A1C (Glycosylated Hemoglobin) for diabetes. But, until we do, we surely shouldn’t put up with politico and admin types who want to generate regulations based on BMI values!
[American College of Sports Medicine (ACSM) 61st Annual Meeting: Abstract 261. Presented May 28, 2014]

