Allergy: Spring Hay Fever and Otherwise
However you spell it: Hay Fever or Hayfever, it’s miserable; and the name has become, like “Kleenex”, the “generic” moniker for any scratchy, itchy, watery red eyes with runny nose – even though the true disease occurs in the fall during the farmer’s haying season.
Hay hauling season: Hay Fever
The more correct names are: Allergic Rhinitis and Allergic Conjuctivitis; but, knowing that, doesn’t make it more tolerable or better treated, they’re all allergy. Those symptoms, for any allergic reasons, are all treated the same whether they are due to hay pollen or tree or weed or mold or… well, you get the picture.
Allergy, Atopy, Hayfever
I think you already must know that inhalant allergies are due to the googolplexian amount of pollen, dust, particles, spores etc. spewed out into the atmosphere by all the plants and other little life-forms.
In a person “blessed” with atopy (the ability to become allergic) the pollen makes a persons mast cells (a type of blood cell) degranulate thereby releasing “inflammatory mediators” – like histamine and other chemicals.
It’s the “mediators” which cause noses to itch and sneeze, eyes to water and itch, noses to drip, sinuses to fill up and throats to scratch and itch. Mucous membranes swell and grow thicker leading to loss of smell and taste AND those same mediators trigger asthma in the lungs too. When the lungs do the same thing that the nose is doing, it’s called bronchospasm and it’s of no small consequence.
Seasonal Allergy
The type of the allergen is what causes the seasonality of a persons symptoms: Dog, cat, chicken and other “danders” are around all the time so the symptoms are year round. Most tree’s pollinate in the spring so that’s when tree-pollen allergies occur. But, as you know, there is a lot of geographical and climate variability in that too (from February to mid-June in most places); California Olive’s in late March and April; Texas Juniper in December through February.
Allergy Methods and Treatment
Only those people who are able to make “allergy antibodies” (immunoglobulin E [IgE]) to the tree’s pollen will mount an allergic reaction. Not everybody can and that’s why it occurs in only certain individuals – 17.6 million people in the United States have been diagnosed with hay fever… at last count… lucky us!
Pollen wafts in and merely touches a mucous membrane where thousands of mast cells reside, they degranulate, inflammatory mediators spew out into the tissues and the blood which carries them to other distant tissues and organs – and all the dripping, clogging, itching and wheezing begins!
When the air is full of allergy triggers, rain helps slam them into the ground and mitigate symptoms. Showering does the same thing in your local environment as does an “electrostatic precipitator” (electronic micro-particle filter.)
Medications the doctor will use include anti-histamines, nasal corticosteroids, inhalant corticosteroids, antihistamine eye drops and mast cell stabilizers; all of which help mitigate the symptoms even though they don’t/can’t “cure” the disease.
We’ve already said that atopy (allergic predisposition) is hereditary; so, if one parent has allergies, children are likely to have them also. If two parents have allergies the likelihood increases significantly.
Spring-Summer Seasonal Allergy Triggers
- Birch
- Beech
- Ash
- Cedar
- Olive
- Juniper
- Sycamore
- Red alder
- Oak
- Pine
- Poplar
- Cottonwood
- Hickory
- Box elder
- Maple
The allergy specialist has a real job on their hands trying to diagnose any specific triggers. The allergy tests, which we’ll discuss below, are expensive and variable; so, the doctor who has a good handle on horticulture has a distinct advantage.
Many allergists have a “station” on the roof of their building with something like “sticky tape” in an open box with only a roof to keep the rain out. Pollen wafting by in the air is captured on the tape where it can be looked at under a microscope and easily identified – at least to someone with experience.
Trees pollinate from late winter to spring, making tree pollen the predominant cause of spring allergies (see table).
The Cedar Fever (caused by the Ashe juniper [Juniperus ashei], shown) has become infamous in Central Texas where it causes wide-spread symptoms in December and January – and even into March.
- Bermuda
- Rye
- Orchard
- Fescue
- Kentucky bluegrass
- Redtop
- Sweet vernal
- Timothy
Grasses, on the other hand, usually pollinate during late spring and summer so their symptoms occur during that time.
They, for some reason I’ve never discovered, seem to me to be the stronger of the two, perhaps due to more “intimate” and frequent contact.
The major grass types throughout the United States include those listed in the second box.
Timothy grass, being the most frequent cause of allergy in most places in the US, is also pictured.
Fall-Winter Seasonal Allergy Triggers
That leads us to the fall-winter types of allergy. You understand that we’re talking about the same disease here, don’t you? Just different triggers for different seasons.
Fall is rife with weeds everywhere; AND, clearly about three-fourths of all the weed pollen burden we experience in the US comes from: Ragweed! Ambrosia artemisiifolia, to be precise (also pictured).
- Lamb’s quarters
- Pigweed
- Russian thistle
- Sagebrush
- Cocklebur
- Plantain
- Mugwort
- Ragweed
Just one ragweed plant can produce 1 BILLION pollen grains – and they never come alone, those suckers run in packs! This is the plant that you can almost see spewing pollen. And you don’t want to park your car next to them when they do it.
Molds, on the other hand, don’t seem to have a regular “season” as such. Instead, their “sporing” is climate dependent. They grow in dark, damp places such as rotting logs and fallen leaves; but, can inhabit basically every space on earth and have adapted to dry, cold, airless and other extreme climates as well.
Thus they don’t have a season but await a particular “climate” change – one which they’ve adapted to in order to facilitate their life-cycle. Dryness, breeziness, humidity, fog and dew all fit the bill.
- Alternaria
- Cladosporium
- Penicillium
- Aspergillus
- Epicoccum
- Fusarium
- Mucor
- Rhizopus
I’ve also listed a few of the major allergy-inducing molds as well.
Allergic Conjunctivitis
Sometimes confused with “Pink Eye” (a bacterial or viral cause) Allergic Conjunctivitis has much the same red, puffy look but is more itchy, less “mattery,” more transient, more recurrent and caused by environmental allergens.
Why bother with the semantics? Well, it’s because they are treated differently and won’t get better if given the other’s medicine.
Those Mast Cells again, come in contact with pollen/spores in the air, degranulation and… well, we’ve gone through this before. The reaction can be prevented (lessened) by anti-histamines either in oral pills or eye drops. Drops can contain antihistamines, mast cell stabilizers or both (dual-action).
Antihistamines found in eye drops include ketotifen, azelastine, olopatadine, and epinastine; mast cell stabilizers include pemirolast and lodoxamide.
Distinguishing Allergies and Viruses
Hayfever vs. a “cold” Although having similar symptoms, both of these have different lengths and timing of symptoms. Caused usually by a Rhinovirus, a cold usually lasts a predictable 7 – 10 days and has a fever with associated feelings of “yukkyness.” They do recur but only sporadically.
Allergies, on the other hand, recur due to season or climate, last longer than 10 days and “yuckyness” is concentrated in the nose and eyes and not throughout the body. After a few episodes of recurrent allergies, the person is usually able to tell the difference if they are thinking about it.
Allergic asthma vs. viral bronchitis/bronchiolitis Again similar symptoms but different timings and causes. X-rays in asthma show over-inflated lungs and physical exam reveals wheezing due to airway narrowing. Both recur but asthma doesn’t usually get better on it’s own (unless season or environment changes). Both have cough and chest tightness but asthma has much more difficulty with breathing and, like above, has less “body yuckyness” than a cold. It “hurts” in the lungs/chest a child will tell you and not so much in the body.
Viruses and bacteria usually have a fever, allergies usually do not. And there are subtle differences on physical exam that a doctor can use in addition to both radiographs and blood tests.
Complications of Inadequate Allergy Treatment
There are risks to NOT treating allergies as well as inadequately treating them with home/internet/quackery remedies.
Poorly treated Allergic Rhinitis can result in Chronic or acute sinusitis, Otitis media, Sleep disturbances, Chronic fatigue, Recurrent Headaches and Throat irritations.
There is also evidence that, if not controlled, allergic rhinitis in the nose and head can even worsen inflammation related to asthma down in the lungs. And, we all know that chronic congestion of any kind will lead to ear infections (Otitis Media) with their often needing surgical intervention.
Allergy Testing
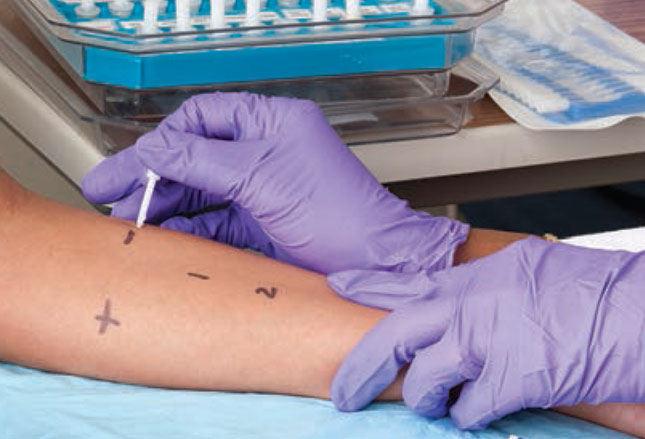
Testing can be done by a couple different methods but the most commonly used, and least expensive, is the “skin testing” method. And it’s the one which has been the longest used.
That’s where the skin (back or arm) is lightly pricked with a “stylus” and a tiny drop of many possible offending antigens is placed on the scratch. Ostensibly, the mast cells residing there will react to the drops that they’ve been causing all the misery about. Problem is that there are millions of possible tests and only one body so the doctor MUST take an extensive history in order to decide which ones to test for – hoping, of course, that he doesn’t miss any important one.
A “wheel and flare” response might develop to antigens from trees, grass, weeds, dust mites, cat/dog dander and/or mold.
Lately, the radioallergosorbent test (RAST) was developed which uses a blood test. Those, however, take several days to be finished, involve taking blood AND are much, much more expensive; which makes them unable to be used to test for very many antigens and more likely to miss some specific ones unique to an individual.
Over-The-Counter (OTC) Medicines For Allergy
Thankfully, the FDA (US Food and Drug Administration) has released some non-sedating antihistamines and corticosteroids into the public, non-prescription marketplace.
Medicines you can purchase OTC include: Antihistamines – Fexofenadine, Loratadine and Cetirizine; and, Nasal Corticosteroids – fluticasone and triamcinolone.
Risks of Some Treatments
Decongestants are also used to treat allergies but you need to be aware that decongestant sprays such as those containing oxymetazoline can actually cause inflammation, runny nose (rhinitis medicamentosa) and bleeding if used for more than a few (like two or three) days.
Pseudoephedrine, a decongestant, is often taken as a pill or liquid but with caution because it will also raise the blood pressure and can cause high blood pressure.
the safest and cheapest of all is to irrigate the nasal passages and sinuses with physiologic saline (salt water of correct concentration) placed in a plastic syringe or rinse bottle.
Allergy Shots
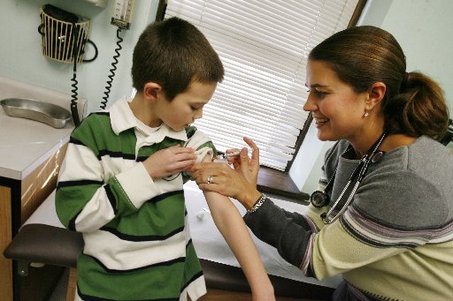
Also known as immunotherapy, a commonly used follow-up to the allergy tests mentioned above is to mix a vial containing miniscule amounts of those antigens which were found to cause reactions and which correlate with the persons symptoms.
Initially, patients start out with the most tiny of doses but week by week, shot by shot the strength is increased until a “maintenance dose” is reached.
All these injections are thought to work by causing the body to additionally make “blocking antibodies” to those antigens in the form of IgG4 and T-regs (regulatory T cells).
Bottom line is that the body’s immune system can then respond to those antigens rapidly and aggressively enough to prevent the “normal” activation of the cascade of events the pesky Mast Cells start off.
The usual course of allergy shots: takes around 3-5 years, does eventually make a difference, sometimes needs a bit of “tweaking” if a specific antigen has been “missed” in initial diagnosis, is a bit cost’y and does (rarely) give an anaphylactic event – which is why patients are asked to remain under observation for 15-30 minutes after each shot.
In 2014 a new under-the-tongue (SLIT) tablet was developed and released which was determined to be at least as effective as immunotherapy FOR SOME GRASS pollens (sweet vernal, orchard, timothy, Kentucky blue and perennial rye).
Because they are more convenient, they are priced by the pharmaceutical industry more expensive than the alternative. And, because of the possible profit, additional SLIT products are under development and production.
Allergy Prevention
This is a bit of a misnomer because there is no way to completely prevent allergies unless you count genetic engineering or other parent choice methods.
We do control the environment however to minimize impact of allergens in five basic ways:
Five Ways To “Control” Allergies
- Limit exposure to pollen and other allergens. Selectively remain indoors, remove/prevent growth of offending plants/animals in your control.
- Keep windows closed, air purifiers for home/car (morning counts are usually highest).
- In cars, set the A/C to “recirculate mode” preventing outside air from entering.
- Appropriately use preventive medications.
- See physician for additional help.
There you have it — whew!