Adolescent Gyn or Pelvic Exams
Recent advances in disease testing methods as well as research into contraception and infection issues has recently prompted a review and adjustment to guidelines for adolescent gyn or pelvic exams.
Technology advances reduce indications for pelvic exams
A gyn exam, involving the external genitalia will have been performed several times before an adolescent completes puberty. A pelvic exam, however, hasn’t been felt necessary until either contraceptives, sexual activity or infection became a concern.
New Gyn Exam Guidelines
Good physicians will perform an examination of the external genitalia on all their patients not only to confirm normal anatomy but to asses pubertal development and look for evidence of abnormal lesions, infection and trauma. Cheap and fairly easy, the pelvic exam has been not only the best method for diagnosis but really the only method available.
The pelvic exam is still a crucial part of the medical evaluation, whose goals are not only to identify diseases and abnormalities early but also to provide education about gynecologic issues and reassure the patient about normal, continued healthy anatomy which they can obtain no other way.
However, technology has progressed such that laboratory tests can now do pretty much the same job as an exam as far as and infections and initiation of birth control pills are concerned. Still fairly easy but not so cheap, these tests still require a vaginal swap be obtained and urine specimens.
Initiating or Maintaining Contraceptives
The guidelines we have used, well pretty much since the things were invented, were fairly easy to follow. Prior to prescribing hormonal contraception, it has been automatic to perform a full pelvic examination to obtain Pap tests and STI testing which may present findings that would contraindicate or modify hormone therapy.
Now, with only a couple exceptions, we have had enough experience to tell with some confidence that a speculum or bimanual exam is not necessary prior to initiating most forms of contraception.
 Pelvic exam and beginning contraceptivesThe reasoning is we now understand that, for the most part, there is nothing found, exclusively on the pelvic exam, which would be a contraindication to a physician prescribing oral contraceptive pills, patch, ring, progestin-releasing implant or medroxyprogesterone injections.
Pelvic exam and beginning contraceptivesThe reasoning is we now understand that, for the most part, there is nothing found, exclusively on the pelvic exam, which would be a contraindication to a physician prescribing oral contraceptive pills, patch, ring, progestin-releasing implant or medroxyprogesterone injections.
What can be used instead, to make sure a pregnancy doesn’t already exist, is a urine based pregnancy test. And to rule out existing infections, one of the several new STI screens can be used.
There are TWO EXCEPTIONS which are: initiating an intrauterine device (IUD) and a diaphragm. In those instances anatomic variation could affect insertion or appropriate sizing of the device so a pelvic exam should be performed before committing to inserting those devices.
Adolescent Sexual Activity and Infections
At the institution of sexual activity by an adolescent female, prevention of pregnancy is NOT the only reason there has been for performing a pelvic exam – infection from a number of organisms and viruses as well as screening for cervical cancer has been and still is a concern.
We now know that cervical cancer generally develops several decades after initial exposure to the human papillomavirus (HPV) and it is rare in women younger than 21 years of age. So now, the guidelines have changed to: perform the first Pap test at age 21, except if a patient has immune suppression or infection with HIV, in which case annual Pap tests are started with the onset of sexual activity.
Adolescents with documented cervical intraepithelial neoplasia (CIN) 2 or 3 or carcinoma found on prior screening still require continued screening according to the new guidelines.
Two other issues went into the new guidelines; namely, we now understand that even though there are many sexually active adolescents exposed to HPV, and even though some develop abnormal cervical cells, those changes mostly resolve without intervention in the majority of cases. Additionally, there is some evidence that interventions in those marginal cases have the potential to contribute to pregnancy complications in the future.
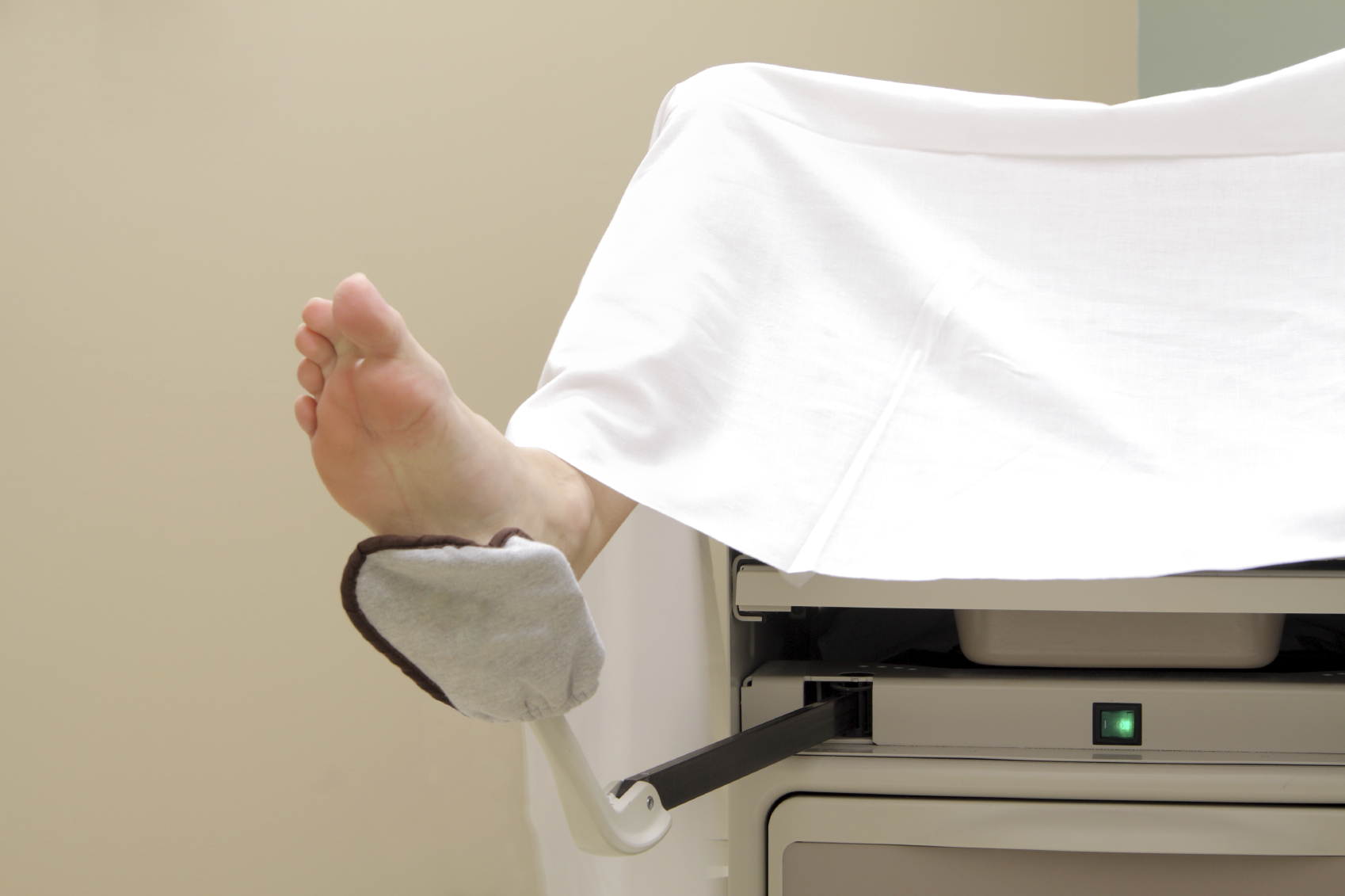 Therefore, now routine pelvic exams are scheduled to begin at age 21 and screening for infections are mostly handled by an external exam with cervical swabs, blood work and urine specimens.
Therefore, now routine pelvic exams are scheduled to begin at age 21 and screening for infections are mostly handled by an external exam with cervical swabs, blood work and urine specimens.
Exceptions and Indications
Numerous indications still remain for a pelvic exam in adolescentsEven though guidelines have changed for speculum and bi-manual exams in birth control and cancer screening, that still leaves many indications for the procedures such as in the case of suspected or reported rape or sexual abuse and/or as part of the evaluation of lower abdominal pain.
In the case of lower abdominal pain, the examination is performed to identify the source of pain, which may be caused by pelvic inflammatory disease, ovarian mass or torsion, and/or normal or ectopic pregnancy.
A speculum exam is also usually performed in the instance where there is persistent symptomatic vaginal discharge. There are complicated tests (NAATs) which can be done on urine samples but cervical or vaginal specimens are usually more sensitive in identifying Chlamydia and Neisseria (gonorrhea). If there is mucopurulent discharge and friability seen at the cervix there is a high likelihood of these diseases even without laboratory testing.
Visualization using a speculum is also important for ruling out other causes of discharge, such as a foreign body or a cervical abnormality such as a large ectropion.
Additionally, there is an indication for a complete pelvic exam in the case of menstrual disorders; such as: dysmenorrhea unresponsive to nonsteroidal anti-inflammatory drugs (NSAIDS) or hormonal therapy; amenorrhea; and abnormal vaginal bleeding.
In these conditions it is important to confirm normal anatomy, isolate the source of pain, rule out lesions or masses, and identify sources of vaginal/uterine bleeding – these require a pelvic exam.
A complete pelvic examination with a speculum may not be necessary for all adolescents with abnormal vaginal bleeding if it is determined that the clinical scenario is that of an individual with heavy and/or prolonged menses within the first few years after menarche who promptly responds to medical management and does not have any indication of trauma or history of sexual activity or abuse.
Some Indications for a Pelvic Examination
- Persistent vaginal discharge
- Dysuria or urinary tract symptoms in a sexually active female
- Dysmenorrhea unresponsive to non-steroidal anti-inflammatory drugs
- Amenorrhea
- Abnormal vaginal bleeding
- Lower abdominal pain
- Contraceptive counseling for an intrauterine device or diaphragm
- Perform Pap test
- Suspected/reported rape or sexual abuse
- Pregnancy
Advertisement by Google
(sorry, only few pages have ads)

